| ABOUT THE AUTHOR | |
 | Dr. Shah practices with Retina Consultants of Houston and is with the Department of Ophthalmology, Blanton Eye Institute, The Methodist Hospital, Houston. DISCLOSURES: Dr. Shah has no relationships to disclose. |
While some of these technologies remain in the early experimental phase, use of WF photography and FA have already led to significant changes in the ability to monitor and evaluate the peripheral retina. Here we review the current literature and highlight the uses of WF imaging.
Widefield Imaging Systems
Widefield imaging systems generally fall into two categories: either portable or office-based. The RetCam (Clarity Medical Systems) is a commonly used portable system. Such portable systems are valuable for screening in neonatal intensive care units for retinopathy of prematurity (ROP) and can be used to examine the peripheral retina in pediatric patients under anesthesia.Office-based systems can include those that use optional contact/noncontact widefield lenses to modify standard fundus photography, such as the Spectralis system (Heidelberg Engineering). However, some imaging systems are exclusively designed for widefield use, such as the 200Tx and Daytona systems by Optos. These cameras can produce a 200° view compared to the 75° view when using overlapping seven standard stereoscopic fields based on the Early Treatment for Diabetic Retinopathy Study (ETDRS) protocols.1,2
WF Imaging in Pediatric Retina
The greatest impact of WF imaging has been in pediatric retina. ROP surveillance with RetCam has proved so effective that many centers utilize nurse practitioners to capture images, which the screening ophthalmologist then reviews (Figure 1). This approach had been validated as early as 2001 and has since been replicated.3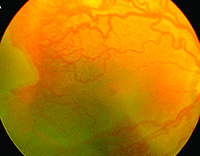 | 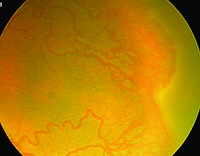 |
| Figure 1. RetCam images of a premature infant screened for retinopathy of prematurity (ROP) show stage 3 ROP in zone 1 (A) and more peripheral stage 3 ROP in zone 2 (B). | |
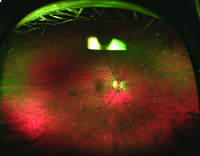 | 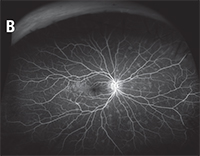 |
| Figure 2. Optos widefield images of a patient with multiple evanescent white dot syndrome. The color fundus photo demonstrates multiple focal gray/white lesions in the posterior pole and, more extensively, in the periphery (A). Similar findings are more apparent on fluorescein angiography with notable late-phase staining (B). | |
Finally, WF imaging has been useful to obtain fundus photography when the patient is too young to cooperate fully and/or diseases such as persistent fetal vasculature syndrome, Norrie disease and Coats’ disease require evaluating peripheral pathology.
Applications in Uveitis
WF imaging has been helpful to identify and monitor the extent of disease in uveitic patients, particularly those with peripheral lesions or retinal vasculitis, has been helpful. In multiple evanescent white dot syndrome, multi-modality imaging makes the extent of peripheral pathology more evident (Figure 2).A small, consecutive case series of four patients with retinal vasculitis that compared conventional FA based on ETDRS protocols to WF FA found that conventional FA could not visualize the full extent of vasculitis and capillary occlusion in any fields.5 While the diagnosis of retinal vasculitis was established, the underlying etiology was not determined in all but one patient diagnosed with Vogt-Koyanagi-Harada disease. Notably, the study found conventional FA would not have detected the posterior extent of vasculitis in two cases.
More recent work has evaluated uveitic patients using widefield FA to describe novel methods for quantifying peripheral vascular pathology to identify visually significant parameters.6 Variables such as peripheral ischemia, peripheral non-perfusion and peripheral leakage, which previously could not be quantified, can now be studied to look for diagnostic and prognostic implications.6
Uses in Ocular Oncology
Retina specialists frequently use WF photography to monitor choroidal nevi and choroidal melanoma for growth, as well as to evaluate edges of plaque-treated choroidal melanomas for recurrence. Multiple modality imaging can be particularly effective in ocular oncology. For instance, WF autofluorescence contrasted against fundus photos can often be used to identify subtle development of orange pigment in choroidal nevi.Other applications of WF photography in ocular oncology under investigation include monitoring mimicking diagnoses such as peripheral exudative hemorrhagic choroidopathy7 and retinal pigment epithelium adenomas.8
WF Imaging and AMD
Retinal specialists have seen significant impact where WF FA has been broadly applied in the study of age-related macular degeneration (AMD),9 central serous chorioretinopathy (CSR)10 and pathologic myopia.11 In AMD specifically, use of other WF modalities such as autofluorescence has detected significant changes in the periphery that are more common in neovascular AMD compared to non-neovascular AMD or normal patients.9 Clinically, WF FA has also been useful to identify the extent of vascular compromise in arterial and venous occlusive diseases.Clinicians have increasingly used this imaging modality in diabetic retinopathy because ETDRS protocol fundus photography can miss the true extent of peripheral non-perfusion and neovascularization (Figure 3).12,13 More recent research has focused on evaluating the role of ischemia in the periphery and its implications and relationship with diabetic retinopathy and ischemia within the macula.14 Research targeting these relationships remains ongoing.
More Studies Are Needed
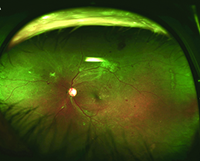 | 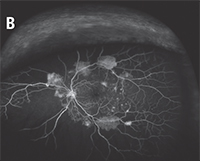 |
| Figure 3. Optos color photos demonstrating extensive neovascularization consistent with proliferative diabetic retinopathy (A). The true extent of the capillary non-perfusion seen on widefield fluorescein angiography would have been missed with standard seven-field montage images (B). | |
A recent study evaluating the retinal periphery in eyes with epiretinal membranes and choroidal nevi, used as surrogates for “normal” retinal periphery, revealed a high prevalence of peripheral vascular anatomic variations. These included vessels crossing the horizontal raphe, right-angle vessels, terminal networks, absence of capillary details, ground glass hyperfluorescence, peripheral drusen and microaneurysms.16 Anton Orlin, MD, and colleagues nicely described a set of 33 control eyes in a study of white without pressure, but some of those controls had conditions (uveitis, vein occlusions and myopia) that have been associated with peripheral changes.17
The literature on normal retinal peripheral vascular anatomy will likely continue to grow and serve as a reference base for future studies examining the pathologic angiographic features of the peripheral retina.
| Take-home Point |
| Portable and office-based systems have made widefield imaging with fluorescein angiography and retinal photography widely available. This has improved the ability of retina specialists to more accurately evaluate pathology, especially in the peripheral retina, in a variety of diseases, including retinopathy of prematurity, uveitis, ocular cancer and age-related macular degeneration. |
Conclusion
As experience with WF imaging grows, so does awareness of peripheral findings in a broad range of retinal pathologies. Only recently have we begun to analyze the retinal periphery in normal patients to establish a meaningful baseline for comparison to the numerous pathologic states currently under study.The future comparison of normal and pathologic populations will be invaluable, particularly as multiple imaging modalities such as color photography, autofluorescence, fluorescein angiography and indocyanine green angiography have recently become available. We remain at the forefront of an imaging revolution within ophthalmology that ultimately should enable better diagnostic testing and monitoring, leading to more effective patient care. RS
References
1. Fundus photographic risk factors for progression of diabetic retinopathy. ETDRS report number 12. Early Treatment Diabetic Retinopathy Study Research Group. Ophthalmology. 1991;98(5 Suppl):823-833.
2. Silva PS, Cavallerano JD, Sun JK, et al. Nonmydriatic ultrawide field retinal imaging compared with dilated standard 7-field 35-mm photography and retinal specialist examination for evaluation of diabetic retinopathy. Am J Ophthalmol 2012;154:549-559 e2.
3. Photographic Screening for Retinopathy of Prematurity (Photo-ROP) Cooperative Group. The photographic screening for retinopathy of prematurity study (photo-ROP). Primary outcomes. Retina. 2008;28(3 Suppl):S47-54.
4. Kashani AH, Learned D, Nudleman E, et al. High prevalence of peripheral retinal vascular anomalies in family members of patients with familial exudative vitreoretinopathy. Ophthalmology. 2014;121:262-268.
5. Hong BK, Nazari Khanamiri H, Rao NA. Role of ultra-widefield fluorescein angiography in the management of uveitis. Can J Ophthalmol. 2013;48:489-493.
6. Karampelas M, Sim DA, Chu C, et al. Quantitative analysis of peripheral vasculitis, ischemia, and vascular leakage in uveitis using ultra-widefield fluorescein angiography. Am J Ophthalmol. 2015;159:1161-1168 e1.
7. Tsui I, Jain A, Shah S, et al. Ultra-widefield imaging of peripheral exudative hemorrhagic chorioretinopathy. Semin Ophthalmol. 2009;24:25-28.
8. Shah SP, Jain A, Coffee RE, McCannel TA. Optos Panoramic 200MA ultrawide-field imaging of peripheral RPE adenoma. Semin Ophthalmol. 2009;24:37-39.
9. Tan CS, Heussen F, Sadda SR. Peripheral autofluorescence and clinical findings in neovascular and non-neovascular age-related macular degeneration. Ophthalmology. 2013;120:1271-1277.
10. Pang CE, Shah VP, Sarraf D, Freund KB. Ultra-widefield imaging with autofluorescence and indocyanine green angiography in central serous chorioretinopathy. Am J Ophthalmol. 2014;158:362-371 e2.
11. Kaneko Y, Moriyama M, Hirahara S, et al. Areas of nonperfusion in peripheral retina of eyes with pathologic myopia detected by ultra-widefield fluorescein angiography. Invest Ophthalmol Vis Sci. 2014;55:1432-1439.
12. Kernt M, Pinter F, Hadi I, et al. [Diabetic retinopathy: comparison of the diagnostic features of ultra-widefield scanning laser ophthalmoscopy Optomap with ETDRS 7-field fundus photography]. Ophthalmologe 2011;108:117-123.
13. Patel RD, Messner LV, Teitelbaum B, et al. Characterization of ischemic index using ultra-widefield fluorescein angiography in patients with focal and diffuse recalcitrant diabetic macular edema. Am J Ophthalmol. 2013;155:1038-4194 e2.
14. Sim DA, Keane PA, Rajendram R, et al. Patterns of peripheral retinal and central macula ischemia in diabetic retinopathy as evaluated by ultra-widefield fluorescein angiography. Am J Ophthalmol. 2014;158:144-153 e1.
15. Yannuzzi LA, Rohrer KT, Tindel LJ, et al. Fluorescein angiography complication survey. Ophthalmology. 1986;93:611-617.
16. Shah AR, Abbey AM, Yonekawa Y, et al. Widefield fluorescein angiography in patients without peripheral disease: A study of normal peripheral findings. Retina. 2015. [In-Press]
17. Orlin A, Fatoo A, Ehrlich J, et al. Ultra-widefield fluorescein angiography of white without pressure. Clin Ophthalmol. 2013;7:959-964.
2. Silva PS, Cavallerano JD, Sun JK, et al. Nonmydriatic ultrawide field retinal imaging compared with dilated standard 7-field 35-mm photography and retinal specialist examination for evaluation of diabetic retinopathy. Am J Ophthalmol 2012;154:549-559 e2.
3. Photographic Screening for Retinopathy of Prematurity (Photo-ROP) Cooperative Group. The photographic screening for retinopathy of prematurity study (photo-ROP). Primary outcomes. Retina. 2008;28(3 Suppl):S47-54.
4. Kashani AH, Learned D, Nudleman E, et al. High prevalence of peripheral retinal vascular anomalies in family members of patients with familial exudative vitreoretinopathy. Ophthalmology. 2014;121:262-268.
5. Hong BK, Nazari Khanamiri H, Rao NA. Role of ultra-widefield fluorescein angiography in the management of uveitis. Can J Ophthalmol. 2013;48:489-493.
6. Karampelas M, Sim DA, Chu C, et al. Quantitative analysis of peripheral vasculitis, ischemia, and vascular leakage in uveitis using ultra-widefield fluorescein angiography. Am J Ophthalmol. 2015;159:1161-1168 e1.
7. Tsui I, Jain A, Shah S, et al. Ultra-widefield imaging of peripheral exudative hemorrhagic chorioretinopathy. Semin Ophthalmol. 2009;24:25-28.
8. Shah SP, Jain A, Coffee RE, McCannel TA. Optos Panoramic 200MA ultrawide-field imaging of peripheral RPE adenoma. Semin Ophthalmol. 2009;24:37-39.
9. Tan CS, Heussen F, Sadda SR. Peripheral autofluorescence and clinical findings in neovascular and non-neovascular age-related macular degeneration. Ophthalmology. 2013;120:1271-1277.
10. Pang CE, Shah VP, Sarraf D, Freund KB. Ultra-widefield imaging with autofluorescence and indocyanine green angiography in central serous chorioretinopathy. Am J Ophthalmol. 2014;158:362-371 e2.
11. Kaneko Y, Moriyama M, Hirahara S, et al. Areas of nonperfusion in peripheral retina of eyes with pathologic myopia detected by ultra-widefield fluorescein angiography. Invest Ophthalmol Vis Sci. 2014;55:1432-1439.
12. Kernt M, Pinter F, Hadi I, et al. [Diabetic retinopathy: comparison of the diagnostic features of ultra-widefield scanning laser ophthalmoscopy Optomap with ETDRS 7-field fundus photography]. Ophthalmologe 2011;108:117-123.
13. Patel RD, Messner LV, Teitelbaum B, et al. Characterization of ischemic index using ultra-widefield fluorescein angiography in patients with focal and diffuse recalcitrant diabetic macular edema. Am J Ophthalmol. 2013;155:1038-4194 e2.
14. Sim DA, Keane PA, Rajendram R, et al. Patterns of peripheral retinal and central macula ischemia in diabetic retinopathy as evaluated by ultra-widefield fluorescein angiography. Am J Ophthalmol. 2014;158:144-153 e1.
15. Yannuzzi LA, Rohrer KT, Tindel LJ, et al. Fluorescein angiography complication survey. Ophthalmology. 1986;93:611-617.
16. Shah AR, Abbey AM, Yonekawa Y, et al. Widefield fluorescein angiography in patients without peripheral disease: A study of normal peripheral findings. Retina. 2015. [In-Press]
17. Orlin A, Fatoo A, Ehrlich J, et al. Ultra-widefield fluorescein angiography of white without pressure. Clin Ophthalmol. 2013;7:959-964.



