 |
History and Examination
The patient is a practicing pharmacist who emigrated from Vietnam to the United States in her late teens. Her ocular history is significant for -9.00 to -10.00 D of myopia in each eye and is status post-bilateral LASIK. Her medical history is significant for tuberculosis (TB) with a positive purified protein derivative (PPD) test and chest X-ray findings, and she is status post-systemic treatment for three to four months.
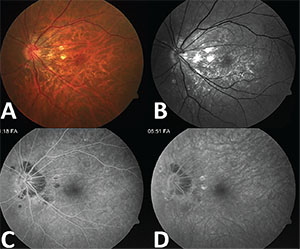 |
| Figure 1. Fundus photo (A) and red-free image (B) of the left eye with peripapillary punched-out lesions. Fluorescein angiography shows early blockage and late hyperfluorescence/staining (C) consistent with multifocal choroiditis (D). |
On exam, visual acuity was 20/30 in the right eye and 20/25 in the left. Intraocular pressures, pupils and anterior segment examination were unremarkable. Dilated fundus examination demonstrated bilateral trace vitreous cell, bilateral peripapillary atrophy and peripheral lattice degeneration OU. Gray lesions superonasal to the disc were in the right eye, and depigmented scars in the left eye.
Macular optical coherence tomography on this initial visit was normal. Fluorescein angiography (FA) demonstrated lesions with blockage in the right eye and lesions with early blockage and late staining in the left eye (Figure 1).
Given the clinical history and findings, we were concerned for multifocal choroiditis (MFC) secondary to TB. We started the patient on four-drug anti-TB therapy as well as oral corticosteroids with close follow-up.
Three months after initial presentation, the patient reported acute worsening of vision in her right eye with 20/200 visual acuity. Repeat examination demonstrated new intraretinal hemorrhage in the macula of the right eye (Figure 2A and B), subretinal hyper-reflectivity with trace subretinal fluid on OCT (Figure 3A) and leakage in the fovea on repeat FA consistent with choroidal neovascularization (CNV) (Figure 2C and D).
Given the development of CNV, we initiated intravitreal bevacizumab (Avastin, Genentech) therapy.1 After three monthly injections, the subretinal fluid resolved on OCT and visual acuity improved to 20/20 (Figure 3 B, page 18). The patient completed a nine-month course of TB treatment started during her initial visit but was then lost to follow-up.
Diagnostic Difficulties
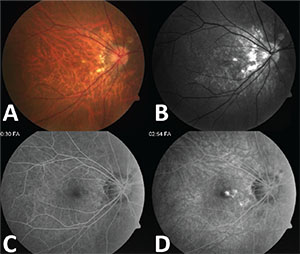 |
| Figure 2. Fundus photo of the right eye on follow-up with parafoveal hemorrhage (A) and red-free image with small parafoveal blockage (B). Early (C) and late (D) fluorescein angiography show late fovea-involving leakage consistent with choroidal neovascularization. |
CNV can be associated with decreased visual acuity or metamorphopsia secondary to subretinal or intraretinal accumulation of fluid, blood or lipid. The pathogenesis of CNV involves ingrowth of vessels from the choriocapillaris into the sub-pigment epithelial space with proliferation between the RPE and Bruch’s membrane (type I) or between the RPE and photoreceptors (type II).
The differential diagnosis for CNV is broad and includes many etiologies, including age-related macular degeneration, pathologic myopia, angioid streaks and chorioretinal inflammatory conditions (i.e., presumed ocular histoplasmosis, MFC, multifocal evanescent white-dot syndrome and punctate inner choroidopathy). CNV may also be idiopathic.2
This case illustrates CNV either secondary to MFC from intraocular TB or pathologic myopia. Though the treatment of CNV is fairly standardized regardless of the etiology, identifying an underlying and treatable etiology, if present, is critical to prevent further episodes or complications.
Intraocular tuberculosis represents a diagnostic dilemma due to variations in presentation. Clinical symptoms, indirect systemic evidence including a positive PPD test or Quantiferon Gold and chest X-ray, the absence of other causes and a positive therapeutic trial suggest presumed ocular tuberculosis. Direct examination of ocular fluids by microscopic analyses, cultures and molecular techniques such as polymerase chain reaction can assist in a definitive diagnosis and provide rationale to initiate anti-tuberculosis treatment.3
High myopia is defined as more than -6.00 D or axial length greater than 26.5 mm, while pathologic myopia is defined as high myopia associated with typical fundus changes described later. Pathologic myopia is the most common cause of CNV in patients younger than 50 years and the second most common cause of CNV overall.
CNV may develop in 5 to 10 percent of eyes with an axial length greater than 26.5 mm. Findings associated with high myopia may include peripapillary crescents, disc tilting, posterior staphylomas and lacquer cracks.2 FA can be helpful in the detection of lacquer cracks and identification of leakage associated with CNV. OCT in these cases of myopic CNV typically demonstrates hyper-reflective lesions with normal overlying retina, but intraretinal fluid, subretinal fluid and RPE detachment may also be observed.
Treatment Options
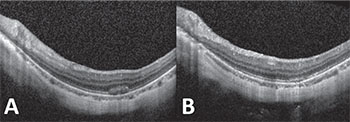 |
| Figure 3. Optical coherence tomography of the left eye with representative subretinal hemorrhage before (A) and six weeks after (B) intravitreal anti-VEGF injection demonstrating resolution of subretinal hemorrhage and responsiveness to therapy. |
The standard treatment for TB includes a four-drug regimen (isoniazid, rifampin, pyrazinamide and ethambutol) for a two-month induction phase followed by four months of rifampin and isoniazid.4 Prolonging treatment is considered under certain circumstances, and accommodations must also be made for multidrug-resistant TB. The addition of corticosteroids for intraocular TB may limit damage secondary to inflammation, but it should not be initiated in the absence of anti-tuberculosis treatment.3 Treatment for CNV secondary to TB includes standard anti-VEGF therapy, modeled on the treatment of CNV secondary to AMD.
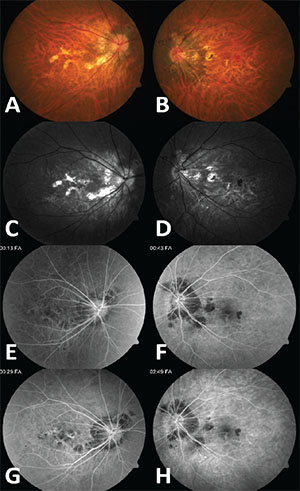 |
| Figure 4. Fundus photos of the right (A) and left (B) eyes and red-free image of the right (C) and left (D) eyes from a more recent visit demonstrate bilateral, macula-involving chorioretinal atrophy compared to initial evaluation seven years prior (Figures 1 and 2) and a small amount of intraretinal hemorrhage in the left eye. Early fluorescein angiography (FA) of the right (E) and left (F) eyes and late FA of the right (G) and left (H) eyes demonstrate window defects and staining in the right eye and window defects and blockage in the left. |
Treatment strategies for CNV secondary to myopic degeneration have included laser photocoagulation, photodynamic therapy and intravitreal anti-VEGF injections. The use of these therapies is extrapolated from studies evaluating the treatment of CNV in AMD. Photocoagulation is of limited utility when lesions involve the fovea and rates of CNV recurrence are high.5 Photodynamic therapy enables treatment of sub-foveal lesions, but it has been associated with decreased visual acuity, retinal atrophy and recurrence.6 In contrast, prospective studies of anti-VEGF injections have demonstrated efficacy and safety.1 Myopic CNV responds exquisitely to anti-VEGF therapy; a single intravitreal injection followed by PRN treatment is comparable to three monthly injections followed by as-needed injections.7
Patient Follow-up
Over the course of seven years, this patient continued to develop recurrent and new CNV in both eyes, which responded to anti-VEGF treatment. Given these recurrent episodes, she underwent an additional nine months of four-drug therapy for TB, thus completing three separate TB treatments in total. She continued to require intravitreal anti-VEGF on a PRN basis.
On her most recent follow-up visit, the patient had excellent visual acuity of 20/30 OU. Fundus examination demonstrated progressive chorioretinal atrophy compared to her initial evaluation seven years prior and a small intraretinal hemorrhage in the left eye (Figure 4 A–D, page 20).
FA demonstrated bilateral window defects, staining more prominent in the right eye than the left and blockage from the hemorrhage in the left eye (Figure 4E–H).
This case represents a diagnostic dilemma in that both TB and high myopia can produce secondary CNV that is clinically indistinguishable. It is possible the complex interplay between these two created a unique clinical entity. Fortunately, with continued treatment of both her TB and her CNV, she has been able to maintain excellent visual acuity. RS
REFERENCES
1. Heier JS, Brown D, Ciulla T, et al. Ranibizumab for choroidal neovascularization secondary to causes other than age-related macular degeneration: A phase I clinical trial. Ophthalmology. 2011;118:111-118.
2. Ryan S. Retina. 5th ed. Philadelphia, PA: Elsevier; 2012.
3. Gupta V, Gupta A, Rao NA. Intraocular tuberculosis—an update. Surv Ophthalmol. 2007;52:561-587.
4. Longo DL, Horsburgh CR, Barry CE, Lange C. Treatment of tuberculosis. N Engl J Med. 2015;373:2149-2160.
5. Neelam K, Cheung CMG, Ohno-Matsui K, Lai TYY, Wong TY. Choroidal neovascularization in pathological myopia. Prog Retin Eye Res. 2012;31:495-525.
6. Kang HM, Koh HJ. Ocular risk factors for recurrence of myopic choroidal neovascularization: long-term follow-up study. Retina. 2013;33:1613-1622.
7. Wang E, Chen Y. Intravitreal anti-vascular endothelial growth factor for choroidal neovascularization secondary to pathologic myopia: systematic review and meta-analysis. Retina. 2003;33:1375-1392.



