A 56-year-old woman presented to our clinic for evaluation and second opinion of recurrent rhegmatogenous retinal detachment in her left eye. Four months earlier she went to a community retina specialist with a macula-involving RRD of the left eye that was repaired promptly with pars plana vitrectomy and gas tamponade.
About a month later she noticed a recurrent “curtain” in her left visual field and was found to have a recurrent detachment. She underwent a repeat pars plana vitrectomy with silicone oil tamponade. In this procedure, the retina specialist contemplated adding a scleral buckle, but did not pursue it due to health concerns about this patient having general anesthesia. Over the next month, she reported persistent poor vision. Within a month of her second surgery, she developed severe proliferative vitreoretinopathy with associated recurrence of her retinal detachment.
Examination Findings
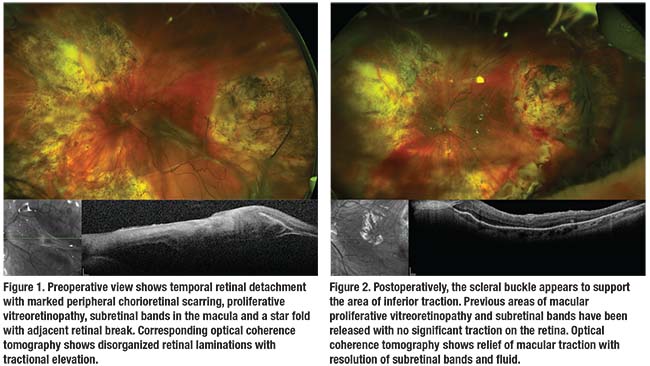
On presentation, visual acuity was found to be bare light perception in the left eye. Intraocular pressure was normal with a left afferent pupillary defect. The anterior segment exam was notable for 3+ milky nuclear sclerotic cataract with posterior synechiae and pigment on the anterior lens capsule. The vitreous cavity had a complete silicone oil fill. The optic nerve appeared normal. A subretinal perfluorooctane (PFO) bubble appeared just nasally to the nerve. The macula was detached with extensive PVR and folds. Large subretinal bands extended into the inferotemporal periphery, where the detachment had recurred. The periphery was notable for significant chorioretinal scarring with a star fold in the 5 o’clock position (Figure 1).
Diagnosis and Management
First, we talked to the patient in detail about the risks and benefits of repeated surgeries for recurrent detachment with PVR. Given her poor visual acuity and history of recurrent detachment, we counseled her on the guarded prognosis for visual recovery in this eye. Ultimately, the patient decided to have the surgery.
The surgical plan included pars plana vitrectomy, pars plana lensectomy, membrane peeling and silicone oil exchange. Although her pathology was concentrated posteriorly in the macula, we also recommended a scleral buckle to reduce anterior-posterior tension on the retina.
In the operating room, a 240-encircling band was placed through four scleral tunnels created 3.5 mm behind the mid-point of the rectus muscle insertions. The buckle was brought to an appropriate height and secured with a 270 sleeve. Iris hooks were placed and a pars plana lensectomy was performed, followed by oil removal.
Upon inspection internally with the wide-angle, non-contact viewing system, we noted the buckle supported the inferotemporal star fold nicely. However, the retina
remained elevated because of contraction of the preretinal membranes and subretinal bands within the macula. We determined the retinal detachment was due to an atrophic break near a chorioretinal scar in the inferotemporal quadrant.
We then peeled the extensive PVR membrane from over the macula and removed the subretinal bands through the pre-existing inferotemporal break. We then performed a retinectomy inferotemporally to relieve the traction from the star fold, using diathermy and the vitreous cutter. Instillation of PFO allowed the retina to flatten fully.
 |
We applied endolaser along the edge of the retinectomy and retinotomy followed by an air-fluid exchange. The retina associated with the retinectomy appeared contracted due to PVR, but the placement of the scleral buckle reduced anterior-posterior tension and allowed for adequate support of the retina. We used 5,000-centistoke oil as a tamponade to fill the vitreous cavity to physiologic pressure.
We instructed the patient to maintain a face-down position for one week. On postoperative day one, her retina was attached without significant subretinal bands or folds (Figure 2).
Over the next month, her retina remained attached under oil and her visual acuity improved from bare light perception to 20/600 (aphakic). She expressed satisfaction with her decision to pursue a third surgical repair.
Discussion
Proliferative vitreoretinopathy is a common obstacle to retinal detachment surgery and accounts for approximately 75 percent of all surgical failures.1,2 Controversy surrounds how to best manage PVR-related detachments. The decision is often based on surgeon preference and expertise.
Pars plana vitrectomy has gained popularity in recent years as a primary method of treating this difficult problem, with several studies showing promising visual and anatomic outcomes.3,4 The use of scleral buckle is typically not employed in these instances because it has been thought to be more useful in cases with primarily anterior pathology.
However, our case demonstrates the utility of using a scleral buckle as an adjunct to vitrectomy to promote anatomical restoration by relieving retinal traction.
Yi Yao, MD, and colleagues in China presented a retrospective non-comparative study evaluating primary scleral buckling for patients with longstanding chronic RRD and subretinal fibrosis.5 Of the 40 eyes studied, the mean duration of detachment was 13.8 months, and four eyes had documented PVR grade C or worse. Anatomical reattachment was achieved in 90 percent of eyes after one procedure and visual acuity improved to better than 5/100 in 77.5 percent of eyes after the final 24- month follow-up.
In a separate study, Philip Storey, MD, and the Wills PVR Study Group compared surgical treatment of 65 eyes at high risk for PVR (retinal detachment in two or more quadrants, retinal tears in one or more clock hour, preoperative PVR or vitreous hemorrhage) with PPV-scleral buckle vs. PPV alone.6 The use of combined PPV-scleral buckle had higher surgical anatomical success relative to PPV alone. However, they found no appreciable difference in visual acuity at three months postoperatively.
In contrast, the European Vitreo-Retinal Society Retinal Detachment Study Group looked at reattachment rates for 637 eyes with grade C PVR RRD.7 Higher anatomical f
 |
ailure rates were associated with combined scleral buckle-PPV (8.9 percent) compared to PPV alone (3 percent), although this result was not statistically significant.
Our patient’s case illustrates an application of scleral buckling to address posterior pathology in a manner that allows a contracted and PVR-affected retina to better adhere to the contour of the eye wall. Although retina surgeons often employ scleral buckling in younger or phakic patients to support anterior pathology,8,9 our case and the cited literature demonstrate its potential utility in cases of severe PVR involving the posterior pole. Further prospective direct head-to-head comparative studies may be useful to determine the role of scleral buckling in such cases. RS
REFERENCES
1. Pastor JC. Proliferative vitreoretinopathy: An overview. Surv Ophthalmol 1998;43:3–18.
2. Campochiaro PA. Pathogenic mechanisms in proliferative vitreoretinopathy. Arch Ophthalmol. 1997;115:237–241.
3. Shah CP, Ho AC, Regillo CD, et al. Short-term outcomes of 25-gauge vitrectomy with silicone oil for repair of complicated retinal detachment. Retina. 2008;28:723–728.
4. Riemann CD, Miller DM, Foster RE, Petersen MR. Outcomes of transconjunctival sutureless 25-gauge vitrectomy with silicone oil infusion. Retina. 2007;27:296–303.
5. Yao Y, Jiang L, Wang Z, Zhang M. Scleral buckling procedures for longstanding or chronic rhegmatogenous retinal detachment with subretinal proliferation. Ophthalmology. 2006;113:821–825.
6. Storey P, Alshareef R, Khuthaila M, et al, for the Wills PVR Study Group. Pars plana vitrectomy and scleral buckle versus pars plana vitrectomy alone for patients with rhegmatogenous retinal detachment at high risk for proliferative vitreoretinopathy. Retina. 2014; 34:1945–1951.
7. Adelman RA, Parnes AJ, Sipperley JO, et al, for the European VitreoRetinal Society (EVRS) Retinal Detachment Study Group. Strategy for the management of complex retinal detachments: the European vitreo-retinal society retinal detachment study report 2. Ophthalmology. 2013;120:1809–1813.
8. Khan MA, Brady CJ, Kaiser RS. Clinical management of proliferative vitreoretinopathy: A review. Retina. 2015;35:165-175.
9. Machemer R, Aaberg TM, Freeman HM, et al. An updated classification of retinal detachment with proliferative vitreoretinopathy. Am J Ophthalmol. 1991;112:159–165.



