Since they first emerged in retinal surgery in the late 1980s,1 perfluorocarbon liquids have become an integral part of our management of complex rhegmatogenous retinal detachments with proliferative vitreoretinopathy2 or giant retinal tears.1–4 More recently, PFCLs have acquired additional, versatile roles in retinal surgery. Here, we provide pearls that we have picked up in training fellows to use PFCLs safely and effectively, and then also explore alternative uses of this versatile fluid.
 |
PFCLs are optically clear and have a specific gravity greater than balanced salt solution (BSS) as well as tensile properties similar to silicone oil but with lower viscosity.1 These properties enable flattening of the retina, unrolling of folds, drainage of subretinal fluid, manipulation of tissues under the liquid and application of endolaser while maintaining good visualization, stabilization of the peripheral retina, and easy injection and removal.
Drs. Yannuzzi, Lin and Sridhar demonstrate their technique for filling the eye with perfluorocarbon liquid in a retinal detachment repair. Watch the video here.
PFCL Pearls for Retinal Detachment Repair
How to Fill
Prior to filling, we make sure that all traction, especially over breaks, has been relieved. We prefer to use a dual-bore cannula to inject PFCL while maintaining a constant intraocular pressure. Alternatively, a single-bore cannula can be used while aspirating fluid through the second trocar with the vitrector or soft tip.
We begin by filling the eye over the attached retina and then fill toward the detached retina (Video). We make sure to aim the cannula away from the fovea when starting the PFCL bubble because too vigorous of an infusion can cause damage to the photoreceptors and commotio retinae, or can open a macular hole.
We try to maintain the cannula in the center of the PFCL bubble when enlarging it to avoid fish eggs. After filling with PFCL, a nice surgical plane may develop to complete a shave of the vitreous base if it hasn’t been performed already. Authors have described accomplishing this by staining with preservative-free triamcinolone acetonide after instilling PFCL to create a vitreous sandwich between a plane of PFCL posteriorly and BSS anteriorly.5
How to Drain
We prefer to fill the PFCL to the most posterior retinal break. Next, we perform a fluid-air exchange while draining from the break. This technique “sandwiches” any residual fluid between the air meniscus and PFCL meniscus (Figure 1). Once the break is dry, we completely remove the PFCL and laser under air.
Another option is to fill the PFCL up to the ora serrata and then laser under the PFCL. However, this maneuver requires an anterior break (or a more anterior edge cut to a posterior break) to prevent retained subretinal fluid (Figure 1). It’s important to note that PFCL drainage may result in trapped subretinal fluid, especially if the SRF is chronic. To facilitate maximal drainage, we rotate the eye to allow the break to assume to the most gravity-dependent area.
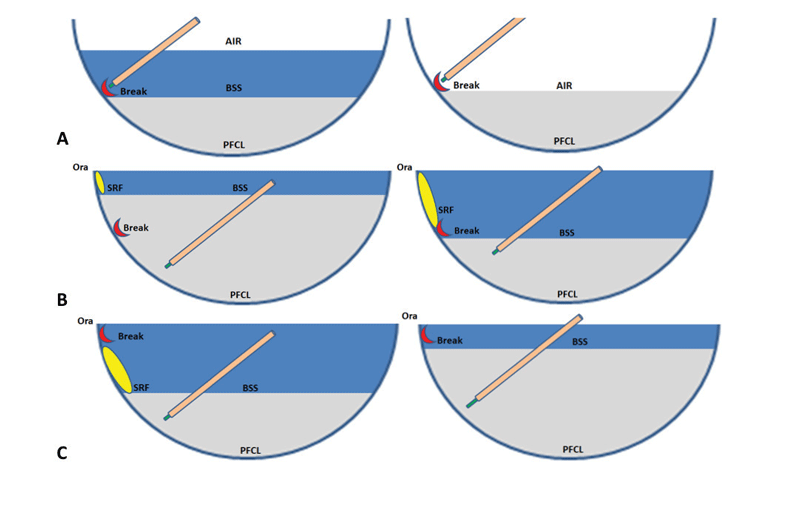 |
Figure 1. Our technique for perfluorocarbon liquid-assisted drainage in rhegmatogenous retinal detachment involves the following steps: A) Fill the PFCL to the most posterior retinal break then perform a fluid-air exchange while draining from the break, “sandwiching” any residual fluid between the air meniscus and PFCL meniscus. B) In the case of a posterior break with extension of anterior fluid, filling PFCL over the break may result in trapping anterior fluid, so one option is to make another retinotomy more anteriorly and then fill to the most anterior iatrogenic break and drain from it. C) In the case of an anterior break located near the ora serrata, PFCL can be filled up to the break without trapping anterior fluid. |
How to Minimize Risk Of Subretinal PFCL And Safely Remove It
Breaks with active traction can act as a sink for PFCL, so we also make sure to relieve any traction before filling and shaving the vitreous gel alongside the bubble. An ophthalmic viscoelastic device (OVD) can also be used to cover retinal breaks while instilling PFCL to prevent subretinal migration in the so-called “soft-shell technique.”6
Fish eggs are a risk factor for subretinal migration, and we try to avoid them in several ways. First, in the case of large retinal breaks we prefer to instill the PFCL through the trocar on the contralateral side to avoid inadvertently introducing bubbles directly into the break. While having an assistant apply depression during shaving at the edge of PFCL, we begin and end the depression slowly and gently to avoid turbulence from rapid changes in the infusion that can cause movement of PFCL into a break.
 |
When removing PFCL, place the tip of the aspirating instrument just within the edge of the PFCL bubble. We teach fellows to maintain a negative pressure gradient on the syringe after filling and after extrusion when exiting the eye to prevent inadvertent dripping of PFCL bubbles from the instrument, especially over the break. During removal of PFCL, this can also be achieved by using a back flush under passive aspiration when entering and exiting the eye. After removing PFCL at the end of the fluid-air exchange, instilling a few drops of BSS over the optic nerve as a “rinse” helps to ensure that no retained vitreous bubble occurs.
Retained PFCL; Now What?
PFCLs can become retained in the anterior chamber and subretinal space (Figure 2). PFCL that has migrated to the anterior chamber can cause visual symptoms, corneal failure and glaucoma. To remove it, a 27-gauge needle can be inserted through the limbus inferiorly and aspirated. Within the retina, PFCL remnants may cause intraocular toxicity, chronic inflammation and decreased retinal sensitivity.7
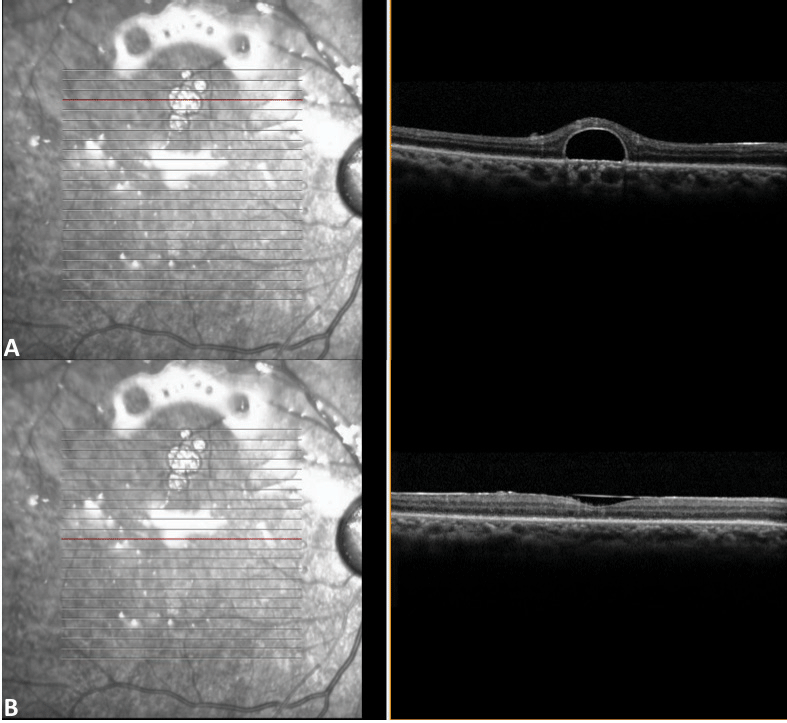 |
| Figure 2. Spectral-domain optical coherence tomography scans of retained subretinal perfluorocarbon fluid in a 52-year-old man with rhegmatogenous retinal detachment repaired by pars plana vitrectomy show two different pictures. Through the superior macula (A), the scan shows several adjacent PFCL bubbles that collected in the subretinal space, as identified by the omega sign on the cross sectional image. Through the fovea (B), the scan shows no evidence of subfoveal PFCL. |
Histopathologic studies have documented macrophages engorged with intracellular vacuoles containing PFCL.8 Subretinal PFCL, when left in the eye for a long duration, may also lead to formation of a retinal hole.9,10 When seen postoperatively and visually significant, submacular PFCL may be displaced by making an inferior retinotomy and injecting BSS through it to form a focal retinal detachment. This allows the fluid to communicate with the retained PFCL. You can then perform a fluid-air exchange to remove the bubble followed by upright head positioning.11
Alternatively, authors have also described direct aspiration of the subretinal PFCL bubble using a 41-gauge needle transretinally.12 Intraoperatively, optical coherence tomography can be used to assist in visualization of retained PFCL and to insure its complete removal.13
Alternative Uses of PFCL
Direct PFCL-to-Silicone Oil Exchange
You may use direct PFCL-to-silicone oil exchange in certain situations with retinal instability, such as a giant retinal tear and retinectomy. To reduce the likelihood of retinal slippage, you can instill PFCL to flatten the retina, after which the infusion line may be connected to a 25-ga oil-infusion cannula and inserted by an assistant, while using the light pipe in one hand and the extrusion line under passive aspiration in the other hand to remove the PFCL as the oil infuses. If operating without an assistant, you can use a chandelier and the 25-ga oil-infusion kit in one hand with the extrusion in the other.14
Lens Fogging
You may encounter lens fogging following the air-fluid exchange, particularly in silicone intraocular lenses. Filling the eye with PFCL to the lens can remove fogging, and laser can be added directly under PFCL.
Ocular Trauma
You can use PFCL to float up a dislocated crystalline lens, dislocated intraocular lens or nonmetallic intraocular foreign bodies.15 PFCL can also help to stabilize metallic foreign bodies, making removal easier.
A cushion of PFCL can also deflect foreign bodies from damaging the posterior pole if dropped during removal.16 A dislocated crystalline lens can be floated anteriorly using PFCL, allowing for a cushion to protect the posterior pole from damage that ultrasound energy, dissipated from the fragmatome, can cause—and also to inhibit subretinal migration of lens fragments. PFCL can also provide countertraction to allow for extraction of foreign bodies enveloped by retina.
Macular Holes
PFCLs can provide a useful interface for endolaser and peeling. However, certain situations may present challenges. For instance, in cases of rhegmatogenous retinal detachment with concurrent macular holes (MH), regrasping an inner limiting membrane flap that is raised and peeled may be difficult because the PFCL bubble will flatten the flap as soon as it is dropped.
Recently, Chirag D. Jhaveri, MD,17 described a novel approach in which a perfluorooctane marble is injected and moved over the macular hole, then the ILM is peeled around it under BSS. This prevents the PFCL bubble from inhibiting flap regrasping but still provides adequate countertraction.
REFERENCES
1. Chang S. Low viscosity liquid fluorochemicals in vitreous surgery. Am J Ophthalmol. 1987;103:
38-43.
2. Coll GE, Chang S, Sun J, Wieland MR, Berrocal MH. Perfluorocarbon liquid in the management of retinal detachment with proliferative vitreoretinopathy. Ophthalmology. 1995;102:630-638; discussion 638-639.
3. Chang S, Lincoff H, Zimmerman NJ, Fuchs W. Giant retinal tears. Surgical techniques and results using perfluorocarbon liquids. Arch Ophthalmol. 1989;107:761-766.
4. Scott IU, Murray TG, Flynn HW Jr, et al. Outcomes and complications associated with giant retinal tear management using perfluoro-n-octane. Ophthalmology. 2002;109:1828-1833.
5. Almeida DR, Chin EK, Roybal CN, Elshatory Y, Gehrs KM. Multiplane peripheral vitreous dissection with perfluoro-n-octane and triamcinolone acetonide. Retina. 2015;35:827-828.
6. Yamakiri K, Uchino E, Sakamoto T. Soft shell technique during vitrectomy for proliferative vitreoretinopathy. Graefes Arch Clin Exp Ophthalmol. 2016;254:1069-1073.
7. Tewari A, Eliott D, Singh CN, et al. Changes in retinal sensitivity from retained subretinal perfluorocarbon liquid. Retina 2009;29:248-250.
8. Elsing SH, Fekrat S, Green WR, et al. Clinicopathologic findings in eyes with retained perfluoro-n-octane liquid. Ophthalmology 2001;108:45-48.
9. Cohen SY, Dubois L, Elmaleh C. Retinal hole as a complication of long-standing subretinal perfluorocarbon liquid. Retina 2006;26:843-844.
10. Tanabu R, Suzuki Y, Suzuki K. Macular hole caused by retained subfoveal perfluorocarbon that subsequently closed after its spontaneous resolution: A case report. Ophthalmol Ther. 2017;6:381-384.
11. Le Tien V, Pierre-Kahn V, Azan F, et al. Displacement of retained subfoveal perfluorocarbon liquid after vitreoretinal surgery. Arch Ophthalmol 2008;126:98-101.
12. Liu W, Gao M, Liang X. Management of subfoveal perfluorocarbon liquid: A review. Ophthalmologica. 2018;240:1-7.
13. Smith AG, Cost BM, Ehlers JP. Intraoperative OCT-assisted subretinal perfluorocarbon liquid removal in the DISCOVER Study. Ophthalmic Surg Lasers Imaging Retina. 2015;46:964-966.
14. Fortun JA, Lakhanpal RR, Berrocal AM, et al. Giant Retinal Tear Repair, A panel discussion with members of the Vit-Buckle Society. Retina Today. 2013;January/February;37-41.
15. Soheilian M, Peyman GA, Wafapoor H, et al. Surgical management of traumatic retinal detachment with perfluorocarbon liquid. The Vitreon Study Group. Int Ophthalmol. 1996;20:241-249.
16. Shah CM, Gentile RC, Mehta MC. Perfluorocarbon liquids’ ability to protect the macula from intraocular dropping of metallic foreign bodies: A model eye study. Retina. 2016;36:1285-1291.
17. Jhaveri CD. PFO marble for macular hole retinal detachment. American Academy of Ophthalmology. Updated April 17, 2017. Available at https://www.aao.org/clinical-video/pfo-marble-macular-hole-retinal-detachments. Accessed August 18, 2018.



