
 |
The development of small-gauge vitrectomy units with high-speed cutters, wide-angle systems and perfluorocarbon liquid has revolutionized the repair of rhegmatogenous retinal detachments and has led to the misconception that scleral buckling surgery is no longer needed in the management of RRD. However, the use of SB surgery remains an essential procedure in RRD management.
One of us (WHR) has operated on 8,903 retinal detachments between 1973 and 2010, 6,216 managed with a scleral buckle alone and 2,687 with a combined pars plana vitrectomy and SB procedure. We make the argument that SB surgery should be the initial procedure performed in phakic patients under 55 years of age who present with RRD.
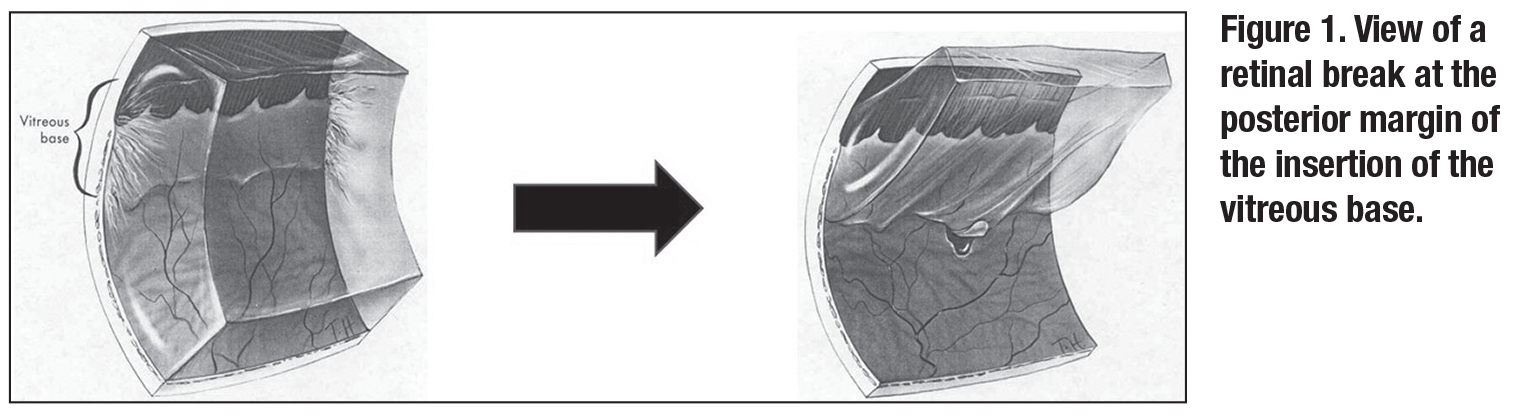
The vast majority of retinal tears are 1 to 3 mm in size and occur at the posterior margin of the insertion of the vitreous base, 3 to 4 mm from the ora serrata. Therefore, a SB that covers 5 to 7 mm of peripheral retina will close most retinal tears (Figure 1).
Here, we review the repair of retinal detachments in phakic younger patients without the presence of proliferative vitreoretinopathy (PVR)—i.e., there are no fixed folds in the detached retina and the retinal tears do not have any rolled edges. Detachments with vitreous hemorrhage that obscure a complete view of the peripheral retina are excluded from this article. The technique we describe does not require drainage of the subretinal fluid.
Surgical planning
Surgical planning begins with a preoperative, peripheral retinal examination with 360-degree scleral depression to find all retinal tears. We perform a retinal drawing to identify all retinal tears and confirm that PVR is not present.
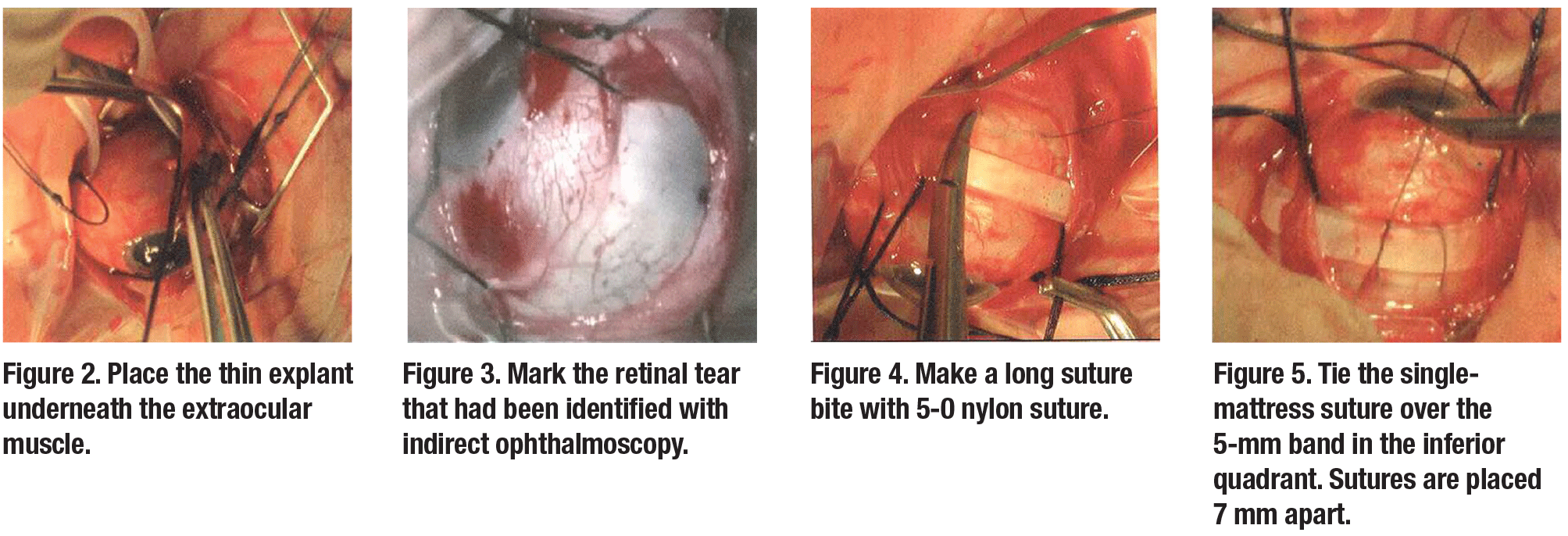
Planning the operation involves selecting the appropriate explant. Explants to repair the detachments have to be wide enough to close the retinal breaks. Explants 3.5 mm (#41), 4 mm (#42) or 5 mm (#5040) in width can be used. The height of the explant would be 0.75 mm (#41), 1 mm (#5040) or 1.25 mm (#42). This thin explant makes it possible to easily pass the explant beneath the extraocular muscles (Figure 2), and will not disturb the function of the muscles by producing diplopia postoperatively. The explant is placed around the eye for 360 degrees to close the original retinal tear and to relieve vitreoretinal traction, to prevent the formation of new retinal tears which would lead to redetachment.
 |
Surgical technique
Modern SB surgery is an external, noninvasive procedure with an operating room time of approximately 30 minutes. It involves the following 15 steps:
1. Administer local retrobulbar anesthesia.
2. Perform conjunctival peritomy for 360 degrees.
3. Hook rectus muscles with 3-0 silk
sutures.
4. Perform indirect ophthalmoscopy to identify and mark all retinal tears (Figure 3).
5. Perform cryopexy of retinal breaks (postoperative laser).
6. Place the band beneath the recti muscles around the globe for 360 degrees.
7. Place 5-0 nylon mattress suture(s) in two inferior quadrants (Figure 4) spaced accordingly:
- 5 mm apart (3.5-mm explant);
- 6.5 mm apart (4-mm explant); or
- 7 mm apart (5-mm explant).
8. Tie 5-1 nylon mattress sutures in the two inferior quadrants (Figure 5).
9. Perform the first anterior chamber tap.
10. Place and tie a 5-0 nylon mattress sutures in the two superior quadrants.
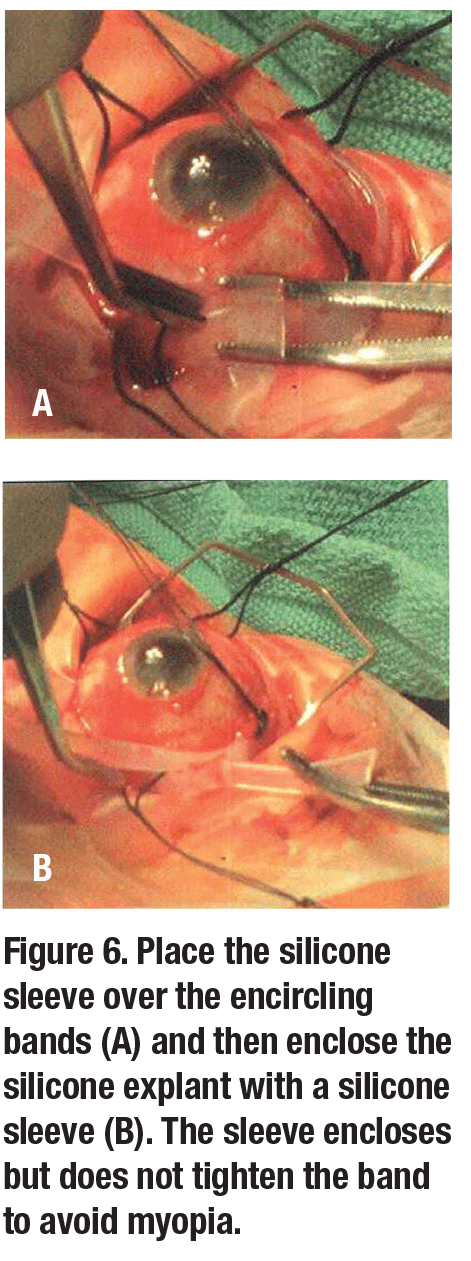
11. Place the silicone sleeve to enclose, not tighten, 5-mm band to avoid myopia (Figure 6 ).
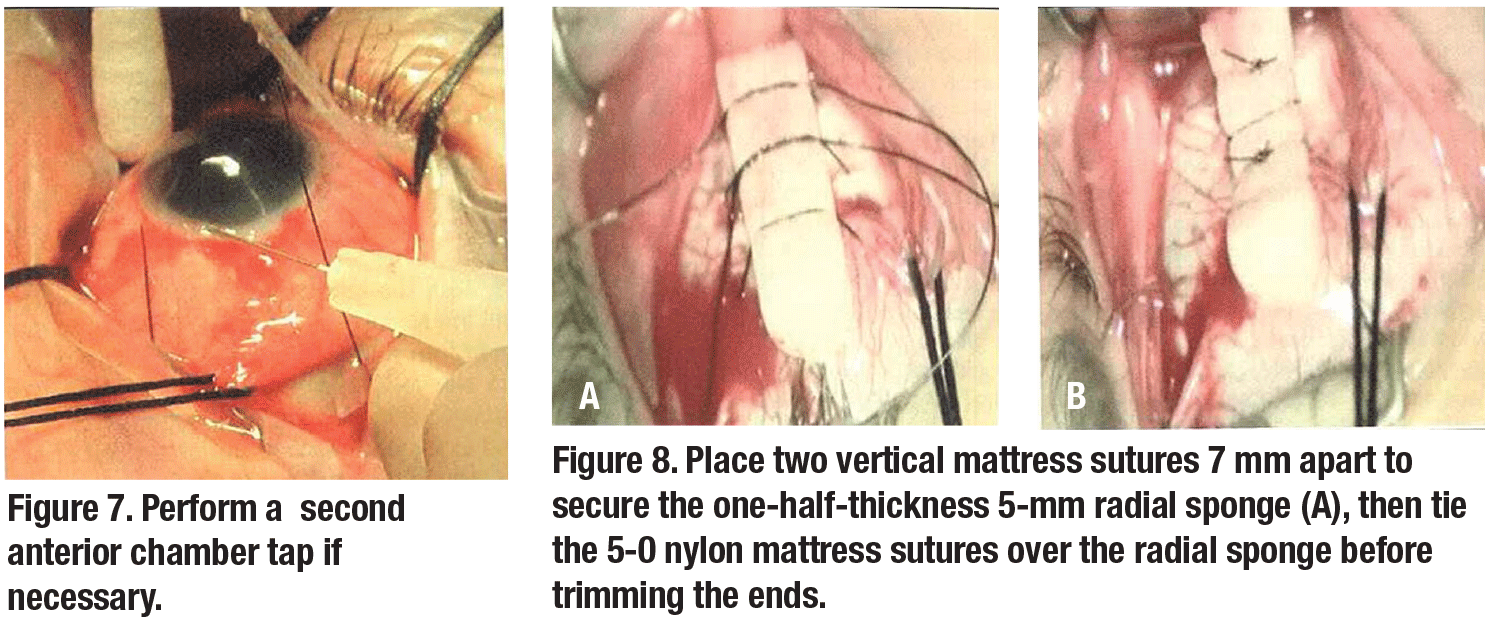
12. Perform the second anterior chamber tap if needed (Figure 7, page 24).
13. Remove the 3-0 silk sutures.
14. Close Tenon’s capsule and conjunctiva with 7-0 vicryl or 6-0 plain gut.
15. Perform indirect ophthalmoscopy to check for central retinal artery pulsations.
Instead of drainage of the subretinal fluid, we use the following steps that allow for tightening of the scleral mattress sutures around the band without increasing intraocular pressure:
- hooking of the recti muscles with 3-0 silk suture;
- cryopexy of the retinal breaks; and
- anterior chamber paracentesis (one or two taps, as needed).
Radial sponges can be extremely useful in the management of retinal detachment secondary to inferior mid-equatorial tears (Figure 8).1
 |
 |
The Value of SB Surgery
This presentation focuses on the management of phakic retinal detachments in younger patients without evidence of PVR. These cases can be successfully managed with an encircling element and without drainage of subretinal fluid, as outlined earlier. These cases represent approximately 50 percent of retinal detachments referred to our clinic for management.
In the remaining 50 percent of patients who present with phakic detachments and associated grade 1 to grade 2 PVR (i.e., fixed folds in one or two quadrants), SB surgery is also indicated. In these cases, a biconvex, segmental buckle 6 or 7 mm wide can be used in one or two quadrants.
Two mattress sutures 7 to 8 mm apart are placed over the solid silicone explant in each quadrant. An encircling 2-mm band is also placed around the globe. Drainage of subretinal fluid beneath the scleral explant can be carried out, followed by injection of SF-6 gas or BSS to restore the volume of the globe and to prevent postoperative myopia. The encircling 2-mm band is simply enclosed in a sleeve without tightening the ends of the 2-mm band to prevent myopia.
The Preference and Trends (PAT) survey of the American Society of Retina Specialists revealed surprising insights into how retina specialists approach phakic RDs.2 When asked how they would manage a hypothetical 45-year-old -3 D myope with a phakic RD, with a one-half clock-hour size flap tear at 6 o’clock anterior to the equator with the macula on and poorer visual acuity in the fellow eye, the survey reported that:
- 58.3 percent would use a primary
buckle; - 21 percent would perform vitrectomy without a buckle; and
- 19.6 percent would perform a vitrectomy with a SB.
What’s alarming is that this type of detachment could easily be managed successfully with a SB procedure without the need of a vitrectomy and its subsequent complications.
 |
Why PnR and SB are still relevant
 |
Many vitreoretinal fellowships no longer emphasize the pneumatic retinopexy (PnR) procedure and SB surgery for RD repair. Virtually all cases undergo PPV. Meanwhile, the majority of patients who present with RD are phakic. The Netherlands study of 2,998 cases revealed that 66.5 percent of
patients who presented with RD were phakic.3 It also demonstrated that the age of patients with the detachments ranged from 55 to 59 years.
The advantages of SB surgery vs. PPV in managing these detachments include:
- No progression of lens opacities that require cataract surgery in one to two years.
- No loss of accommodation in phakic patients following cataract surgery.
- In myopic patients, who represent 35 percent of retinal detachments,4 PPV would result in anisometropia following cataract surgery, requiring the patient to wear a contact lens or undergo a clear lens extraction in the fellow eye.
- No invasion of the vitreous with an increased stimulus for postoperative PVR.
- No restriction on air travel due to gas expansion and elevated IOP following PPV surgery.
- A reattachment rate of 92 to 94 percent, which is comparable to PPV surgery.
- Faster postoperative rehabilitation.
In the 6 to 8 percent of patients for whom buckling surgery is not initially successful, a secondary PPV with the buckle in place would result in a higher reattachment rate.
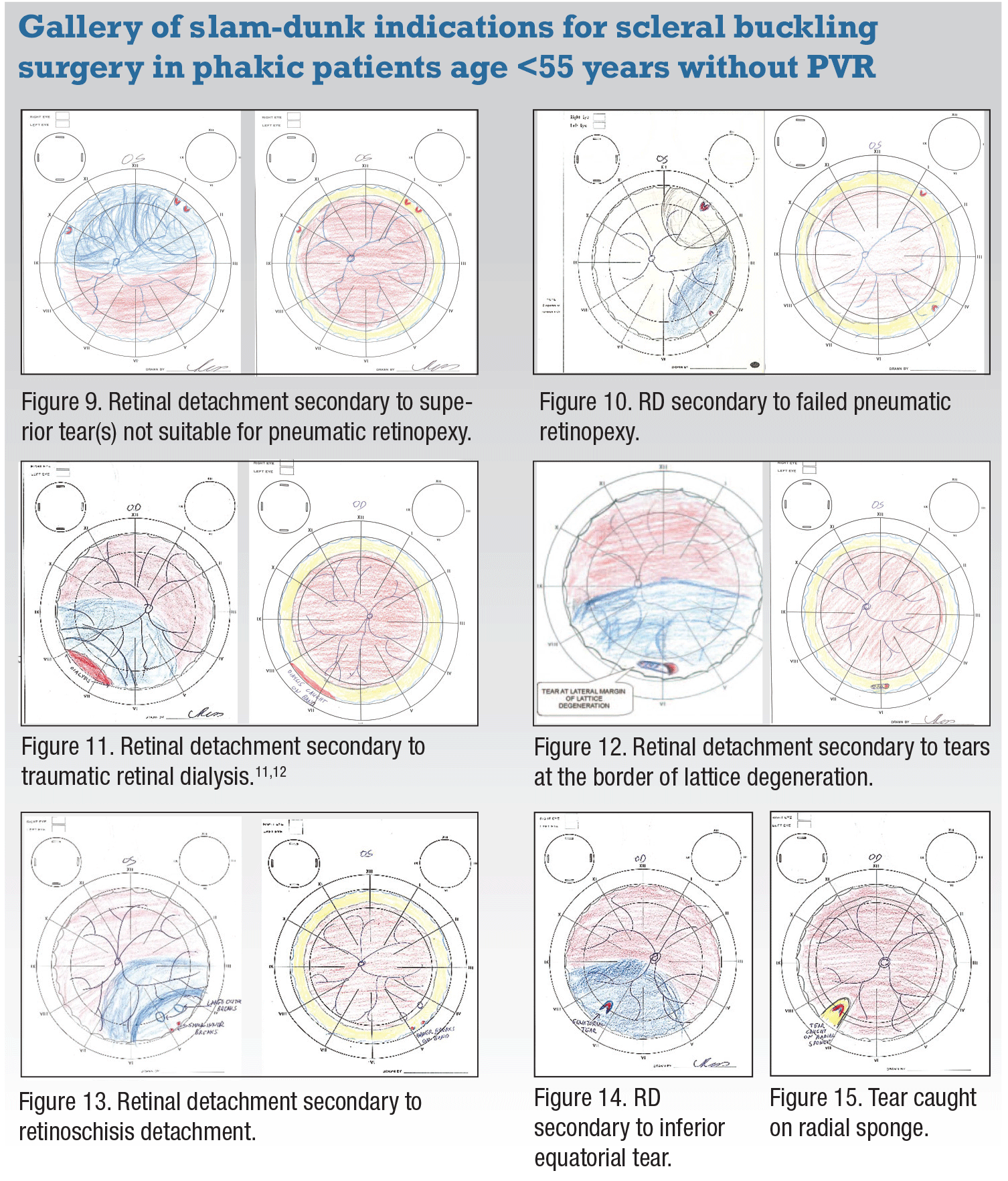 |
Has fellowship training forsaken scleral buckling surgery?
 |
At our institution, each vitreoretinal fellow performs between 120 and 200 PnR procedures and 35 and 70 SB operations during the one-year program. We’ve trained 57 VR fellows since 1986, including 11 from Canada and 29 from the United States. However, we’ve noted that the majority of vitreoretinal fellowships in the United States and abroad don’t adequately teach the value of PnR procedures and SB surgery in the management of phakic RDs. Virtually all patients who present with RDs are managed with PPV, despite evidence that PnR and scleral buckling surgery produce comparable anatomic and visual results.
A recent prospective study by Roxane J. Hillier, MBChB,5 compared pneumatic retinopexies with PPV in the management of phakic RDs. The primary anatomic success at 12 months was achieved in 80.8 percent of patients undergoing PnR vs. 93.2 percent undergoing PPV (p=0.045), with 98.7 and 98.6 percent, respectively, achieving secondary anatomic success. Most importantly, 65 percent of phakic patients in the PPV arm underwent cataract surgery in the study eye within 12 months vs. 16 percent in the PnR group (p<0.001).
A prospective, randomized multicenter clinical study8 reported an equal single-
operation success of 63.6 and 63.8 percent for SB and PPV, respectively, in phakic detachments. In North America, we anticipate a single-operation success rate of approximately 90 percent for both scleral buckling and pars plana vitrectomies.
 |
It’s interesting to speculate why SB surgery is no longer used universally in the management of phakic detachments.7,8 The reason may be that many vitreoretinal fellowships no longer teach SB surgery. It requires properly marking the retinal breaks, placing the scleral sutures and draining the subretinal fluid, if necessary. We strongly believe that teaching the technique of SB surgery in the management of the types of detachments we’ve outlined should be an integral part of any vitreoretinal fellowship.
 |
 |
Treatment plan for phakic RRD
If the RD involves the superior retina between 8 and 4 o’clock, and if the break or group of breaks are no larger than one clock hour (i.e., 30 degrees of detached retina), a PnR procedure should be performed first. We anticipate a success rate of between 70 and 80 percent with a pneumatic procedure.9,10
If the PnR fails, then a scleral buckling procedure should be carried out. This would increase the reattachment rate to between 92 and 94 percent. PPV would be reserved for patients who remained detached following scleral buckling surgery, with a final reattachment rate of 98 to 99 percent.
 |
Bottom line
For inferior retinal detachments, SB surgery is the treatment of choice. It will result in a success rate of 92 to 94 percent. For the 6 to 8 percent of patients in whom SB surgery is unsuccessful, a PPV would then be carried out. PPV will result in a final reattachment rate of 98 to 99 percent.
REFERENCES
1. Ross WH. Radial sponges in retinal detachment surgery. Can J Ophthalmol. 1977;12:268-274.
2. Hahn P. Preferences and trends (PAT) survey 2018. Presented at American Society of Retina Specialists annual meeting; Vancouver, B.C.; July 23, 2018.
3. Van de Put MAJ, Hooymans JMM, Los LI; for the Dutch Rhegmatogenous Retinal Detachment Study Group. The incidence of rhegmatogenous retinal detachment in The Netherlands. Ophthalmology. 2013;120:616-622.
4. Schepens C, Marden BA: Data on the natural history of retinal detachment. Am J Ophthalmol. 1966;61:213-226.
5. Hillier RJ, Felfeli T, Berger AR, et al. The Pneumatic Retinopexy vs. Vitrectomy for the management of Primary Rhegmatogenous Retinal Detachment Outcomes Randomized Trial (PIVOT). Ophthalmology. 2019;126:531-539.
6. Heimann H, Bartz-Schmidt KU, Bornfeld N, Weiss C, Hilgers RD, Foerster MH; for the Scleral Buckling versus Primary Vitrectomy in Rhegmatogenous Retinal Detachment Study Group. Scleral buckling versus primary vitrectomy in rhegmatogenous retinal detachment: A prospective randomized multicenter clinical study. Ophthalmology. 2007;114:2142-2154.
7. D’Amico DJ. Different preferences between United States and European vitreoretinal surgeons: personal observations. Curr Opin Ophthalmol. 2016;27:196-200.
8. Hwang JC. Regional practice patterns for retinal detachment repair in the United States. Am J. Ophthalmol. 2012;153:1125-1128.
9. Hilton GF, Grizzard WS. Pneumatic retinopexy. A two-step outpatient operation without conjunctival incision. Ophthalmology. 1986;93:626-641.
10. Emami-Naeini P, Deaner J, Ali F, et al; for the Academic Vitreoretinal Training Centers Study Group. Pneumatic retinopexy experience and outcomes of vitreoretinal fellows in the United States: A multicenter Study. Ophthalmol Retina. 2019;3:140-145.
11. Ross WH. Traumatic retinal dialysis. Arch Ophthalmol. 1981;99: 1371-1374.
12. Ross WH. Retinal dialysis: Lack of evidence for a genetic cause. Can J Ophthalmol. 1991;26: 309-312.



