 |  |
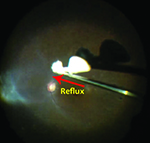 | 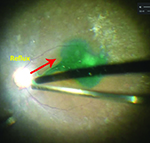 |
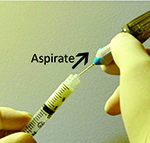
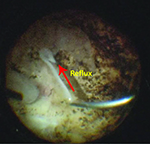
| Reflux chromovitrectomy starts with aspirating the agent into the vitreous cutter (A). Views of reflux Triesence (Alcon) with the hyaloid separated (B) and hyaloid attached (C), and reflux indocyanine green (D). Online video available at http://goo.gl/vVfcPQ. | |
Vitreous Cutter as Injector
To address this challenge, I have developed a technique that I have called “reflux chromovitrectomy.”1 Rather than using a syringe with cannula to inject the chromovitrectomy agent, I now use a standard vitreous cutter.To do this, I ask the nurse to draw up the agent in a syringe in standard fashion. Next, I insert the cutter into the syringe to aspirate a small volume of agent. Then, I insert the cutter into the eye and use the vitrectomy foot pedal to directly reflux the agent into the vitreous cavity (Figure). Immediately, without instrument exchange, I can use the vitreous cutter already in the eye to proceed with the vitrectomy, hyaloid elevation, removal of excess agent or whatever the next step may be.
Taking Precautions
I recommend these three precautionary steps when attempting this maneuver:• To avoid air bubbles, I recommend aspiration of the agent rather than cut/aspiration, and I reflux a small amount first outside the eye.
• Undiluted kenalog does not reflux very smoothly. Diluting kenalog or using undiluted (or diluted) Triesence (Alcon) may be preferable.
• Because of the sideways-facing port of the vitreous cutter, application of dyes on the retinal surface requires turning the port down or allowing additional time for the dye to settle and stain. I dilute my ICG (25 mg) in 20 ml of 5% dextrose in water, and not the diluent included with the product. This facilitates settling. I usually allow it to sit for approximately 15 seconds before I remove it.
With these precautions in mind, I have found this technique to be universally accessible, effective, efficient, easy and surgeon-controlled. It spares the use and cost of additional injection cannulas.
Visualizing Triamcinolone Flow
Visualization of the flow of triamcinolone reflux provides feedback on the vitreous morphology. A stream suggests the hyaloid is syneretic or elevated, while a slow, clumping reflux suggests a formed, usually attached, vitreous (Figure). The sideways-facing port is directional, which allows peripheral application even in phakic patients, minimizes flow directly at the surface of the retina, and can be rotated to direct toxic dyes away from a macular hole or other retinal break.In today’s environment, with increasing pressures toward greater efficiency and lower cost, maximizing multi-functional capabilities is paramount. Current small-gauge vitreous cutters have emerged as the retina specialist’s “Swiss Army Knife,” often replacing the need for secondary instruments.
Reflux is a powerful extension of this multi-functionality, and its capabilities extend beyond refluxing inadvertently engaged retina or dispersing settled heme. “Reflux hydrodissection” can help separate planes in traction retinal detachments.2
I find reflux very useful for diagnostic vitrectomies to cut/aspirate undiluted vitreous samples and reflux them directly into a collection tube, bypassing the need for assistant-controlled (or what I consider to be uncontrolled) aspiration of a connected syringe. For me, using reflux and other multi-functional capabilities is an important step to becoming a better, safer and more efficient surgeon. RS
Dr. Hahn is an assistant professor of ophthalmology at Duke University Eye Center, Durham, N.C. Disclosures: Dr. Hahn serves as a consultant for Second Sight Medical Products and Bausch + Lomb.




