The Early Treatment Diabetic Retinopathy Study (ETDRS) established and refined the current clinical grading of diabetic r
 |
etinopathy that retina specialists use as an adaptation of the Modified Airlie House Classification. The parameters of the grading system rely primarily on identifying somewhat indirect signs of microvascular ischemic disease that include retinal hemorrhages, venous beading, intraretinal microvascular abnormalities or preretinal neovascularization.
However, identifying indirect signs of microvascular disease is fraught with challenges in ensuring reproducibility among different observers and operators, which may introduce error into research or clinical settings. ETDRS made attempts to measure and minimize this variability and found that certain exam features proved to be more reliable than others between independent observers.1
This is similar to what happened before the widespread use of optical coherence tomography to assess diabetic macular edema, when clinicians used biomicroscopy and they based the determination of clinically significant macular edema (CSME) on observed retinal thickening and presence of exudates as defined by ETDRS.
With the advent of OCT and anti-VEGF medications, a more direct approach has emerged. Clinicians can now easily identify macular fluid in cross-section and localize it in relation to the foveal center. They can also measure macular thickness to the nearest micron and easily establish trends between clinic visits.
Potent anti-VEGF agents allow more flexibility and salvage therapy if clinicians observe interval worsening much more rapidly than the previously applied focal/grid laser. In many ways, the enhanced visualization of microanatomy along with rapid advances in treatment have obviated the indirect measures of CSME as the ETDRS study had defined it.
Enter OCTA to Evaluate DR
There is now a growing body of literature applying the more nascent OCT angiography to the classification and management of diabetic retinopathy. Implementing OCTA to directly visualize diabetic microangiography in a far more detailed manner provides additional information about the severity of retinopathy not previously available in the classification scheme defined by ETDRS.
Going forward, understanding the applications of the additional information OCTA provides may similarly change our approach to diabetic retinopathy.
Basis of OCTA
OCT renders cross-sectional images of retinal
 |
tissues in vivo. The original basis of OCT was on time-domain technology that obtained depth-resolved tissue reflectivity characteristics based on the technique of interferometry. This approach takes light backscatter from the examined tissue and compares it to light reflected from a reference mirror. This can render the interference signal into cross-sectional images of the examined tissue once the position of the reference mirror is moved to detect backscattered light from varying depths.2
With technological advancements such as spectral domain and swept source OCT, methodologies that eliminate the need for movement of the reference mirror can detect backscattered signals from biological tissues and increase the acquisition speed. The use of a broader bandwidth light source in these approaches also considerably enhances axial resolution.
Now with improved speed and resolution, detailed three-dimensional images of the examined tissues can be created, allowing for detailed in vivo visualization of retinal and choroidal anatomy. However, the produced images do not differentiate between the static backscattering of light, such as those from the retinal laminations, compared to those that produce variable backscattering of light, such as in the retinal vasculature where varying configurations of red blood cells (RBCs) continually travel.2
 |
Isolating and exhibiting only tissues with variable backscattering of light is the basis of OCTA. By repeating an OCT scan multiple times within the same tissue, algorithms can be applied to isolate only areas that produce variable backscattering of light such as those produced by the continual flux of RBCs through blood vessels.
In the retina, the acquired image isolates functional blood vessels and has clinical applications in conditions that affect vascular tissues, such as DR, choroidal neovascularization, retinal vein occlusion, retinal artery occlusion or uveitis.2
Given that newer OCT technology can rapidly image tissues in a three-dimensional manner, the application of OCTA to these scans allows us to understand microvascular
 |
anatomy like never before. It can render pathology in greater detail.
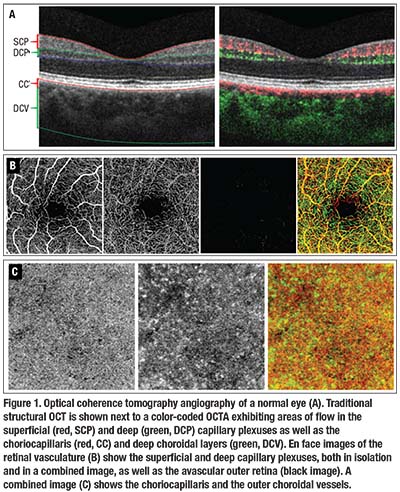
Diseases that previously affected the “retinal circulation” or the “choroidal circulation” on conventional imaging, can now be further localized to the superficial or deep capillary plexuses of the retina or the choriocapillaris or deeper vessels of the choroid (Figure 1, page 21). Recalibrating our approach to conditions such as DR with this additional information will undoubtedly guide future research efforts.
Diabetes Without Clinically Apparent Retinopathy
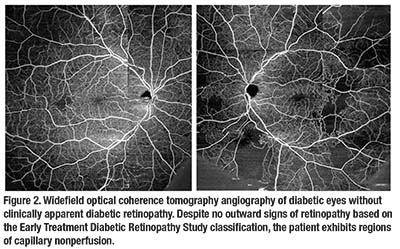
The enhanced imaging of retinal capillaries using OCTA can enable the detection of DR even before clinical signs of mild nonproliferative diabetic retinopathy (NPDR) appear (Figure 2). Noriaki Takase, MD, and colleagues in
 |
Japan found that the foveal avascular zone was larger in both the superficial and deep capillary plexuses of diabetic patients with no clinical signs of diabetic retinopathy (NDR) compared to nondiabetic eyes.3 Talisa de Carlo, MD, and colleagues at New England Eye Center corroborated these findings, and also found that the foveal avascular zone in NDR patients appeared remodeled (36 percent vs. 11 percent, p=0.01) and with higher rates of capillary nonperfusion (21 percent vs. 4 percent, p=0.03) compared to nondiabetic eyes.4
Another study quantified capillary vessel density in the superficial (44.35 percent vs. 51.39 percent, p=0.04) and deep (31.03 percent vs. 41.53 percent with, p<0.01) capillary plexuses, and was found to be less in NDR eyes compared to nondiabetic eyes.5 Furthermore, systolic blood pressure and ocular perfusion pressure correlated significantly with deep capillary plexus density in NDR patients, but not in controls.
Authors have suggested that OCTA may be used in such circumstances to assess the risk of progression of NDR to clinically apparent DR, or even to screen patients for diabetes by observing these early microvascular alterations.
A pilot study has been performed implementing automated computer processing of OCTA images, which demonstrated 94.3 percent accuracy, 97.9 percent sensitivity and 87 percent specificity in detecting DR when analyzing the superficial and deep capillary plexuses.6 The approach may have important implications in primary care and may encourage further emphasis on preventative care.
NPDR
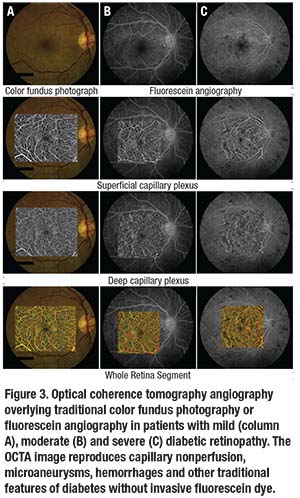
Clinicians can observe the traditional features of clinically apparent diabetic retinopathy with excellent detail using OCTA (Figure 3). However, OCTA also enables examination of DR features that were not previously accessible with traditional imaging modalities, and with far greater detail. For one, we can examine retinal perfusion with higher resolution and with better standardization than we can with fluorescein angiography.
This has allowed quantitative approaches to measure retinal perfusion that were not previously possible. Our group at the University of Washington, led by Alexander D. Lin, MD, calculated the capillary perfusion index, defined as percent coverage of functional retinal capillaries in the traditional ETDRS zones.6
We compared NDR/mild NPDR patients to moderate/severe NPDR patients. The results showed a significantly lower perfusion index in all non-foveal ETDRS zones in the moderate/severe NPDR group, suggesting a correlation between capillary perfusion and severity of diabetic retinopathy.
Kumar Sambhav, MD, and colleagues at the University of Florida College of Medicine, Jacksonville, reported similar results in a prospective
 |
cross-sectional study involving 102 eyes with newly diagnosed NPDR (36 mild NPDR, 21 moderate NPDR, 13 severe NPDR, and 32 with NPDR with DME) and 60 control eyes.7
They reported the following deep parafoveal vessel density measurements:
• 25.23 percent in mild NPDR.
• 20.16 percent in moderate NPDR.
• 11.16 percent in severe NPDR.
• 17.91 percent in NPDR with DME.
Spearman correlation coefficient (rs) showed an inverse correlation between vessel density and NPDR severity in both the superficial (rs -0.87, p=0.083) and deep capillary plexuses (rs -0.96, p=0.017).7
Does OCT Enable More Quantitative Classification?
Given the observed correlations between clinically graded DR and capillary perfusion, it begs the question of whether OCTA may enable a more quantitative classification of DR that may allow for better predictions on progression to proliferative diabetic retinopathy, progression of macular ischemia or response to anti-VEGF therapy.
One study observed that eyes with both greater abnormality and more microaneurysms in the deep capillary plexus, along with larger foveal avascular zones, tended to respond less to anti-VEGF injections for DME than their counterparts.8 Further study is needed to better understand and utilize data on retinal capillary perfusion in NPDR and possibly define quantitative classifications of severity based on OCTA imaging.
Proliferative DR
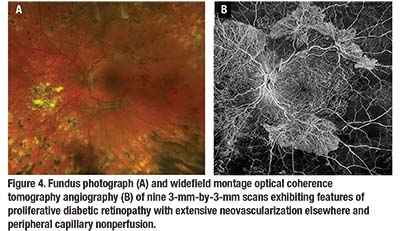
As in NPDR, the degree of retinal capillary perfusion has been correlated to the development of PDR. Peter Nesper, MD, and colleagues at Northwestern University performed an analysis and found linear correlations with the size of the foveal avascular zone, vessel density and percentage of area of nonperfusion. They did this comparing NPDR eyes to PDR eyes using 3-mm-by-3-mm scans centered on the fovea.9 Dr. de Carlo and colleagues were able to create montage images (similar to those in Figure 4) using nine 3-mm-by-3-mm OCTA scans to observe the perfusion status of the retinal periphery.10
The Future of OCTA in DR
Future study is necessary to both standardize and elucidate the applications of widefield OCTA in DR, as the ischemic burden that contributes to the progression to PDR is likely more heavily concentrated in the
retinal periphery rather than the central macula.
OCTA can
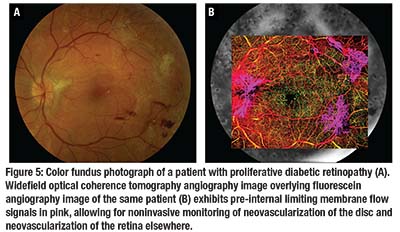 |
directly image the retinal neovascularization that results from capillary nonperfusion, including intraretinal microvascular abnormalities, neovascularization of the disc and neovascularization elsewhere (Figure 5).11 Given that OCTA is noninvasive compared to traditional fluorescein angiography, routine monitoring of neovascular complexes is now possible and may become standard practice, especially as the evidence grows for the treatment of PDR with repeated anti-VEGF medications over traditional panretinal photocoagulation.12–14
Lastly, a growing body of evidence suggests that ocular involvement of diabetes may not be limited to the retina but may also affect the vasculature of the choroid. In one study involving 157 diabetic eyes, choroidal thickness on SS-OCT was on average thinner when compared to 71 normal eyes.15 In another study, choroidal vascular density and volume were significantly reduced in PDR compared to NPDR and control eyes.16
Furthermore, choroidal vascular index—the ratio of the choroid composed of luminal vessel area to total choroidal area on the OCT scan— has been shown to be lower in diabetics compared to healthy controls when imaged with SS-OCT.17 Dr. Nesper and his group used OCTA to show that choriocapillaris vessel density was significantly lower in PDR patients compared to NPDR and NDR patients.9
Another study used OCTA to observe flow voids in the choriocapillaris of 108 eyes of 66 consecutive diabetic patients, which the authors associated with higher severity of diabetic retinopathy and with poorer visual prognosis.18 The role of assessing diabetic choroidopathy with OCTA remains to be seen. RS
Acknowledgment: The authors would like to gratefully acknowledge the lab of Ruikang Wang, PhD, for his contributions to the OCTA images included in this article.
REFERENCES
1. Grading diabetic retinopathy from stereoscopic color fundus photographs--an extension of the modified Airlie House classification. ETDRS report number 10. Early Treatment Diabetic Retinopathy Study Research Group. Ophthalmology. 1991;98(5 Suppl):786-806.
2. Kashani AH, Chen C-L, Gahm JK, et al. Optical coherence tomography angiography: A comprehensive review of current methods and clinical applications. Prog Retin Eye Res. 2017;60:66-100.
3. Takase N, Nozaki M, Kato A, Ozeki H, Yoshida M, Ogura Y. Enlargement of foveal avascular zone in diabetic eyes evaluated by enface optical coherence tomography angiography. Retina. 2015;35:2377-2383.
4. de Carlo TE, Chin AT, Bonini Filho MA, et al. Detection of microvascular changes in eyes of patients with diabetes but not clinical diabetic retinopathy using optical coherence tomography. Retina. 2015;35:2364-2370.
5. Dimitrova G, Chihara E, Takahashi H, Amano H, Okazaki K. Quantitative retinal optical coherence tomography angiography in patients with diabetes without diabetic retinopathy. Invest Ophthalmol Vis Sci. 2017;58:190-196.
6. Lin AD, Lee AY, Zhang Q, et al. Association between OCTbased microangiography perfusion indices and diabetic retinopathy severity. Br J Ophthalmol. 2017;101:960-964.
7. Sambhav K, Abu-Amero KK, Chalam KV. Deep capillary macular perfusion indices obtained with OCT angiography correlate with degree of nonproliferative diabetic retinopathy. Eur J Ophthalmol. March 2017:0. doi:10.5301/ejo.5000948 [Epub ahead of print]
8. Lee J, Moon BG, Cho AR, Yoon YH. Optical coherence tomography angiography of DME and Its association with anti- VEGF treatment response. Ophthalmology. 2016;123:2368- 2375.
9. Nesper PL, Roberts PK, Onishi AC, et al. Quantifying microvascular abnormalities with increasing severity of diabetic retinopathy using optical coherence tomography angiography. Invest Ophthalmol Vis Sci. 2017;58:BIO307-BIO315.
10. de Carlo TE, Salz DA, Waheed NK, Baumal CR, Duker JS, Witkin AJ. Visualization of the retinal vasculature using widefield montage optical coherence tomography angiography. Ophthalmic Surg Lasers Imaging Retina. 2015;46:611-616.
11. de Carlo TE, Bonini Filho MA, Baumal CR, et al. Evaluation of preretinal neovascularization in proliferative diabetic retinopathy using optical coherence tomography angiography.
Ophthalmic Surg Lasers Imaging Retina. 2016;47:115-119.
12. Hutton DW, Stein JD, Bressler NM, et al. Cost-effectiveness of intravitreous ranibizumab compared with panretinal photocoagulation for proliferative diabetic retinopathy:secondary analysis from a Diabetic Retinopathy Clinical Research Network randomized clinical trial. JAMA Ophthalmol. 2017;135:576-584.
13. Writing Committee for the Diabetic Retinopathy Clinical Research Network, Gross JG, Glassman AR, et al. Panretinal photocoagulation vs. intravitreous ranibizumab for proliferative diabetic retinopathy: A randomized clinical trial. JAMA. 2015;314:2137-2146.
14. Li X, Zarbin MA, Bhagat N. Anti-vascular endothelial growth factor injections: The new standard of care in proliferative diabetic retinopathy? Dev Ophthalmol. 2017;60:131-142.
15. Abadia B, Suñen I, Calvo P, Bartol F, Verdes G, Ferreras A. Choroidal thickness measured using swept-source optical coherence tomography is reduced in patients with type 2 diabetes. PloS One. 2018;13:e0191977.
16. Wang JC, Laíns I, Providência J, et al. Diabetic choroidopathy: choroidal vascular density and volume in diabetic retinopathy with swept-source optical coherence tomography. Am J Ophthalmol. 2017;184:75-83.
17. Kim M, Ha MJ, Choi SY, Park Y-H. Choroidal vascularity index in type-2 diabetes analyzed by swept-source optical coherence tomography. Sci Rep. 2018;8:70.
18. Dodo Y, Suzuma K, Ishihara K, et al. Clinical relevance of reduced decorrelation signals in the diabetic inner choroid on optical coherence tomography angiography. Sci Rep. 2017;7:5227.



