 |
|
Bios
Dr. Hsu is with Mid Atlantic Retina/Retina Service, Wills Eye Hospital, Philadelphia, where Dr. Soares is a fellow. DISCLOSURES: Drs. Hsu and Soares have no relevant financial relationships to disclose. |
A 65-year-old woman with a complaint of progressive blurred vision in both eyes for six months was referred to the clinic. She complained that driving at night and walking in the dark had become difficult. Her ocular history was unremarkable.
On further questioning, she reported a medical history significant for Crohn’s disease. She had undergone multiple small-bowel resections, which ultimately led to short-bowel syndrome and loss of a substantial amount of weight three months before her visit. She was not taking any medications. Her family and social history were otherwise unremarkable.
Workup and imaging findings
On presentation, visual acuity was 20/40 in both eyes. Intraocular pressures were normal. The anterior segment was unremarkable bilaterally. Fundus examination revealed multiple yellow-white punctate dots with a granular appearance throughout the posterior pole and mid-periphery in both eyes (Figure 1). The macula exhibited a stippled appearance.
The optic nerves and vasculature were normal in both eyes. Fundus autofluorescence (Figure 2) revealed bilateral stippled hyperautofluorescence. Optical coherence tomography (Figure 3) revealed a jagged ellipsoid zone irregularity with focal hyperreflective excrescences localizing to the spots seen on the fundus examination.
Serum laboratory studies were notable for normal chemistry panel and complete blood count. FTA-ABS/RPR was negative. Testing for zinc was within normal limits. Vitamin A was found to be low at 8.5 (normal >22.9).
The diagnosis is …
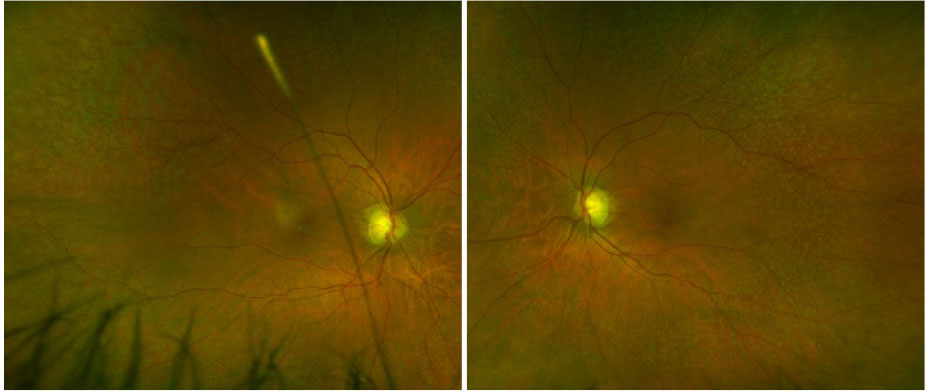 |
| Figure 1. Fundus examination revealed innumerable yellow-white punctate dots throughout the posterior pole and mid-periphery in both eyes. |
We diagnosed vitamin A deficiency retinopathy and referred the patient to her gastroenterologist and primary-care physician, in addition to a nutritionist. She was started on 10,000 IU of oral vitamin A supplementation daily with plans for possible intramuscular injection if her short-gut syndrome precluded vitamin absorption.
Follow-up
Two months after the initial daily supplementation with oral vitamin A, the patient reported an improvement in night vision. Her visual acuity remained stable at 20/40 in both eyes, and the anterior segment remained normal without signs of xerosis. Fundus examination and OCT remained stable.
A disease of malnutrition
Vitamin A is a fat-soluble vitamin found in dairy, meat, fish and leafy green vegetables.1 It’s an essential nutrient for immune function, epithelial cell maintenance and, in the retina, for the production of rhodopsin in rods. Vitamin A deficiency often first affects the visual system by causing night blindness. Later, loss of conjunctival goblet cell function leads to conjunctival and corneal xerosis, manifested by the classic “Bitot spot.”2
Vitamin A deficiency has historically been a disease related to malnutrition, especially in children and breastfeeding women in developing countries. Paradoxically, vitamin A deficiency, once considered rare in developed countries, is increasing in prevalence. As bariatric surgery has become a common solution to morbid obesity, the spectrum of malabsorption syndromes complicating bariatric surgery has led to an increase in the incidence of vitamin A deficiency and night blindness.3–5 Other syndromes and surgical interventions that interfere with vitamin A absorption in the duodenum have also been associated with night blindness.6,7
Role of multi-modal imaging
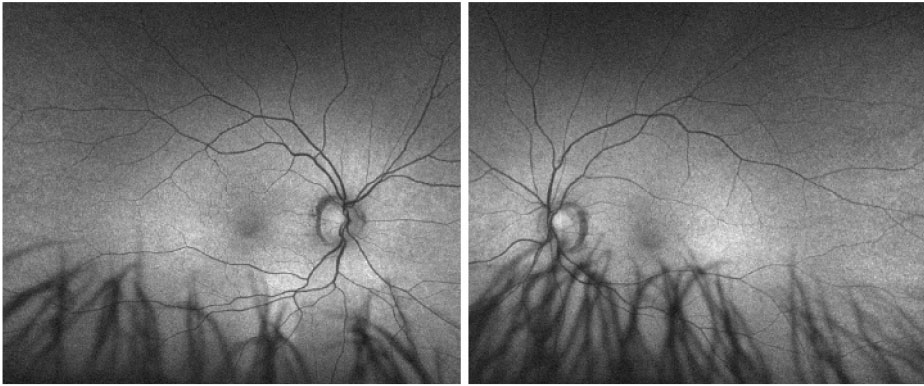 |
| Figure 2. Fundus autofluorescence revealed bilateral stippled hyperautofluorescence correlating to the yellow-white dots on fundus examination. |
Night blindness from vitamin A deficiency doesn’t always present with fundoscopic findings. In some cases the only objective manifestation is peripheral constriction on visual-field testing and diminished scotopic responses on electroretinography.8
Vitamin A deficiency retinopathy, on the other hand, describes patients with fundoscopic disease. Classically, vitamin A retinopathy presents as yellow-white spots that may or may not resolve with treatment.9,10 Some have theorized that these yellow-white dots represent the disruption of the retinoid cycle with subsequent accumulation of photoreceptors underneath the retina but overlying the RPE.11 Such accumulation is thought to “block” autofluorescence, yielding the hypoautofluorescence of these spots reported.11 OCT findings further reveal the hyperreflective deposits under the ellipsoid zone band, again possibly shed photoreceptors.11
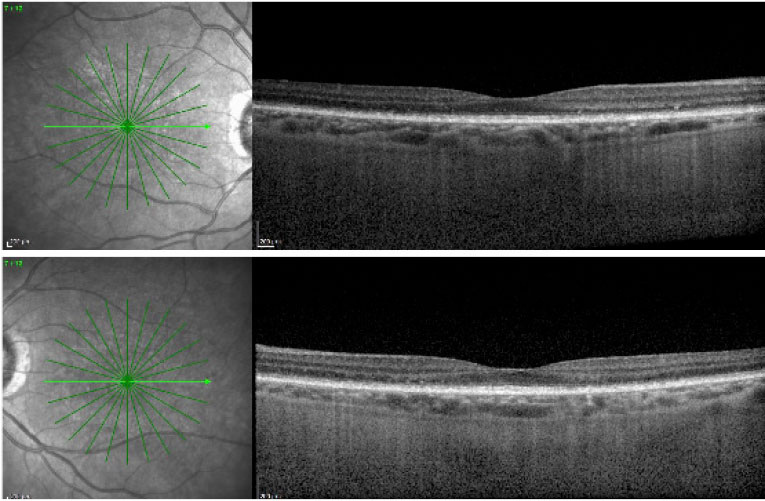 |
| Figure 3. Optical coherence tomography revealed jagged irregularity of the ellipsoid zone with underlying hyperreflective deposits. |
Treatment options
In patients having bariatric surgery or other types of significant small bowel resection, prophylactic supplementation with 5,000 to 10,000 IU of vitamin A daily is recommended to prevent deficiency.12
For adults with night blindness, the World Health Organization similarly recommends a daily oral dose of up to 10,000 IU of vitamin A for at least four weeks. Patients with concomitant severe xeropthalmia should receive 200,000 IU of oral vitamin A daily for two days and then once two weeks later. Those unable to absorb vitamin A should receive intramuscular vitamin A.13
Few case reports characterize the response of the flecked fundus lesions to vitamin A replenishment. Some have found no improvement in the lesions years after supplementation,9 while others find a marked improvement.10 Interestingly, OCT may also show reduced central sub-foveal thickness that resolves with treatment.9 RS
REFERENCES
1. Perusek L, Maeda T. Vitamin A derivatives as treatment options for retinal degenerative diseases. Nutrients 2013;5:2646–2666.
2. World Health Organization. Global prevalence of Vitamin A Deficiency. Micronutrient Deficiency Information System Working Paper No. 2. 1995. Available at: https://www.who.int/nutrition/publications/micronutrients/vitamin_a_deficiency/WHO_NUT_95.3/en/ Accessed November 8, 2020.
3. Slater GH, Ren CJ, Siegel N, et al. Serum fat-soluble vitamin deficiency and abnormal calcium metabolism after malabsorptive bariatric surgery. J Gastrointest Surg Off J Soc Surg Aliment Tract 2004;8:48–55; discussion 54-55.
4. Angrisani L, Santonicola A, Iovino P, et al. Bariatric Surgery Worldwide 2013. Obes Surg 2015;25:1822–1832.
5. Lee WB, Hamilton SM, Harris JP, Schwab IR. Ocular complications of hypovitaminosis a after bariatric surgery. Ophthalmology 2005;112:1031–1034.
6. Cheshire J, Kolli S. Vitamin A deficiency due to chronic malabsorption: An ophthalmic manifestation of a systemic condition. BMJ Case Rep 2017;2017.
7. Parafita-Fernández A, Escalona-Fermín MM, Sampil M, et al. Acquired night blindness due to bad eating patterns. Eur J Clin Nutr 2015;69:752–754.
8. Spits Y, De Laey J-J, Leroy BP. Rapid recovery of night blindness due to obesity surgery after vitamin A repletion therapy. Br J Ophthalmol 2004;88:583–585.
9. Saenz-de-Viteri M, Sádaba LM. Optical coherence tomography assessment before and after vitamin supplementation in a patient with vitamin A deficiency. Medicine (Baltimore). 2016;95:e2680.
10. Apushkin MA, Fishman GA. Improvement in visual function and fundus findings for a patient with vitamin A-deficient retinopathy. Retina. 2005;25:650–652.
11. Aleman TS, Garrity ST, Brucker AJ. Retinal structure in vitamin A deficiency as explored with multimodal imaging. Doc Ophthalmol. 2013;127:239–243.
12. Aasheim ET, Björkman S, Søvik TT, et al. Vitamin status after bariatric surgery: A randomized study of gastric bypass and duodenal switch. Am J Clin Nutr. 2009;90:15–22.
13. World Health Organization. Vitamin A supplements : A guide to their use in the treatment of vitamin A deficiency and xerophthalmia. 1997. Available at: https://apps.who.int/iris/handle/10665/41947 Accessed November 8, 2020.




