View the Video
Drs. Sastry and Grewal demonstrate their technique for diagnostic vitrectomy and retinal biopsy.
Preoperative Evaluation, Prep
Prior to surgery, it is imperative to communicate with the cytopathologist, flow cytometry laboratory and any outside laboratories to determine their preferences for specimen processing, handling and transport. It is also important to have a differential diagnosis to appropriately allocate the higher-quality, undiluted sample to higher-yield studies.
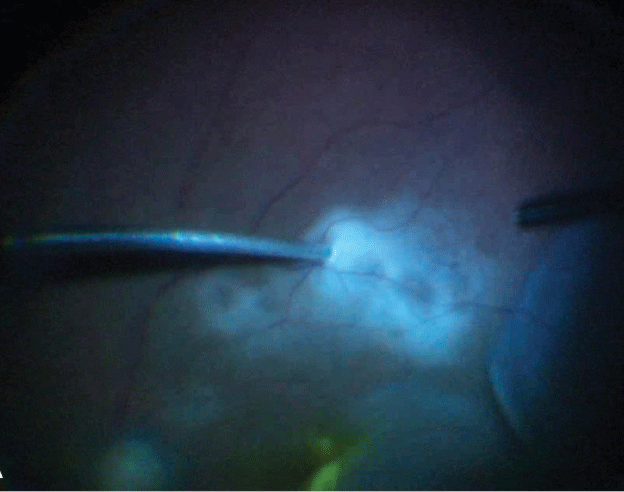 |
| Figure 1. Retinal biopsy is obtained by inserting the tip of a 27-gauge cutter into the lesion. |
On the day of surgery, it’s helpful to pre-label the collection tubes and have them ready on the sterile fi eld. The surgeon personally aliquotes the obtained samples into the tube.
Surgical Technique
1. Connect infusion line. The procedure begins with the infusion line connected to the eye but clamped to avoid premature intraocular dilution. At the Duke Eye Center, where a fellow or other skilled assistant is consistently available, a 10-cc syringe is connected to the disengaged aspiration line of the cutter for manual aspiration.
2. Reduce cut rate. Reducing the cut rate to ~1,000 cpm may minimize morphological alterations in the sample. As you initiate vitreous cutting in the mid-vitreous cavity, an assistant gently aspirates the vitreous using the attached syringe. Undiluted vitrectomy continues until the eye becomes hypotonous. Alternatively, the infusion can be opened to air, which may maximize the volume of an undiluted sample and prevent hypotony.
 |
| Figure 2. Retinal tissue is aspirated into the vitreous cutter tubing confirmed on visualization (black arrows). |
3. Harvest the sample. In the absence of a skilled assistant, a “vitreous trap” uses a vacutainer to provide a simple, surgeon-controlled method for obtaining undiluted samples.1 Alternatively, the undiluted sample can be harvested through a standard vitrectomy setup (i.e., with the aspiration line connected to the vitrectomy machine), followed by either reflux of the obtained sample into a collection tube or aspiration with a syringe from the aspiration line that is disengaged after the sample is collected. This latter technique is probably the simplest, but risks some loss of the precious sample
4. Open infusion line. Following harvesting of the undiluted sample, the infusion line is opened to fluid, and a diluted sample is obtained with a fresh 10-cc syringe. Drs. Sastry and Grewal prefer to aspirate all the diluted sample in 10-cc syringes, which simplifies processing by the lab vs. sending the vitrectomy cassette
5. Aspirate tissue for biopsy. If a retinal biopsy is indicated, a 27-gauge cutter can be directly introduced into the retina or subretinal space (Figure 1) and the tissue aspirated using high vacuum (~600 mmHg) and low cut rate (~300 to 500 cpm). Once you visualize the specimen in the infusion line (Figure 2), withdraw the cutter and reflux the sample into the collection tube (Figure 3). Alternatively, a larger piece of retinal tissue may be harvested using scissors and carefully extracted through an enlarged sclerotomy. In such cases, the retinotomy is barricaded with endolaser. Intraocular tamponade is usually used.
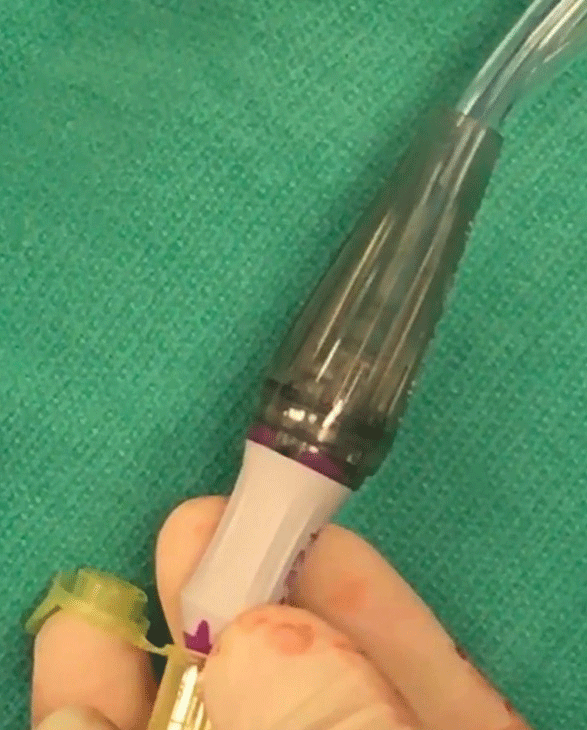 |
| Figure 3. Sample is refluxed from the vitreous cutter tubing directly into the microcentrifuge tube and then sent for analysis. |
While diagnostic vitrectomy and retinal biopsy are the preferred techniques for tissue diagnosis, it’s important to recognize that the yield is dependent upon obtaining a sufficient volume of cells/tissue, choosing appropriate tests and communicating appropriately with the laboratory.
Dr. Sastry is a vitreoretinal surgery fellow and Dr. Grewal is an associate professor of ophthalmology, specializing in vitreoretinal surgery and uveitis, at the Duke Eye Center, Durham, N.C.
Reference
1. Malinowski SM. The vitreous trap: A simple, surgeoncontrolled technique for obtaining undiluted vitreous and subretinal specimens during pars planavitrectomy. Retina. 2010;30:828-829.




